Led by Katie Baldwin, Ph.D., research published in Neuron shows how the loss of the protein hepaCAM drives brain development dysfunction and plays an important role in neurological disorders
CHAPEL HILL, NC – When we think of the brain, we think of neurons. But much of the brain is made of non-neuronal cells called glial cells, which help regulate brain development and function. For the first, time UNC School of Medicine scientist Katie Baldwin, PhD, and colleagues revealed a central role of the glial protein hepaCAM in building the brain and affecting brain function early in life.
The findings, published in Neuron, have implications for better understanding disorders, such as autism, epilepsy, and schizophrenia, and potentially for creating therapeutics for conditions such as the progressive brain disorder megalencephalic leukoencephalopathy with subcortical cysts (MLC).
For over one hundred years, the glia were thought of as a bunch of support cells, like a kind of brain glue keeping the more important neurons in place to do the brain’s real work. But over the past 30 years, scientists have been teasing apart the importance of glial cells as regulators of brain development and function. Still, much remains unknown, especially about complex glial cells called astrocytes, which extend thousands of fine branches throughout the brain, directly interacting with neurons and other brain cells.
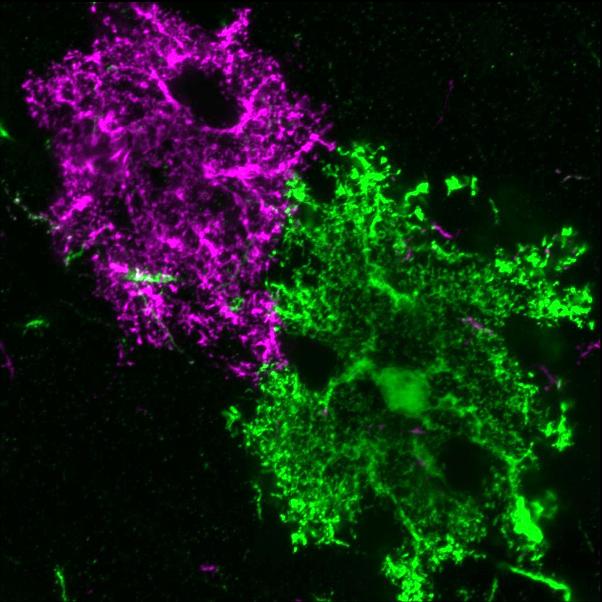
During brain development prior to birth and thereafter, astrocytes establish an intricate network of distinct territories, a sort of tiling of the brain, like the tiles of a soccer ball. These cells use specialized connections, called gap junctions, to communicate throughout this network.
“Both astrocyte tiling and communication through gap junctions are disrupted in different brain disorders and following injury, suggesting these features are important for normal brain function,” said Baldwin, the corresponding author, member of the UNC Neuroscience Center, and assistant professor in the UNC Department of Cell Biology and Physiology. “But prior to our study, it was unknown how astrocytes established their territories and whether there was a link between astrocyte territory and gap junction communication, also known as coupling.”
In this study, Baldwin and colleagues focused on hepaCAM, a protein abundantly expressed on the astrocyte membranes. They created a transgenic rodent model so the animals did not express any hepaCAM protein in astrocytes. The researchers used this model along with cutting-edge genetic and imaging techniques to study the developing astrocytes, their resulting tile-like territories, and gap junction coupling.
“Deleting hepaCAM from astrocytes disrupted astrocyte territories and impaired gap junction coupling. Essentially, these astrocytes no longer do a good job of communicating with their neighbors,” Baldwin said. “We also found that, even though we did not make any disruptions to neurons, loss of hepaCAM in astrocytes altered the balance of synaptic excitation and inhibition.” That is, without this protein, astrocyte branches in contact with neurons affected the how neurons behaved.
“We think our findings have important implications for understanding the pathogenesis of MLC, as well as the general role of astrocyte dysfunction as a driving cause of neurological disorders, such as epilepsy,” Baldwin said.
Baldwin conducted this work while a postdoctoral fellow in Cagla Eroglu’s lab at Duke University before joining UNC-Chapel Hill this past spring. Her lab will continue to focus on the impact of hepaCAM mutations on astrocyte function.
“We are building on this research to explore the bigger question of how astrocytes balance their connections with other cell types in the brain,” she said, “with the goal of understanding how problems in astrocytes cause disease in humans, and how we might help people with these serious and complex disorders.”
###
Other authors of the study are Cagla Eroglu, Christabel Tan, Samuel Strader, Changyu Jiang, Justin Savage, Xabier Elorza-Vidal, Ximena Contreras, Thomas Rülicke, Simon Hippenmeyer, Raul Estevez, and Ru-Rong Ji.
The National Institutes of Health, a Holland Trice Brain Research Award, a Foerster-Bernstein Family Postdoctoral Fellowship, The Hartwell Foundation, and the European Research Council funded this research.
Media Contact
Mark Derewicz
[email protected]
Original Source
https:/
Related Journal Article
http://dx.