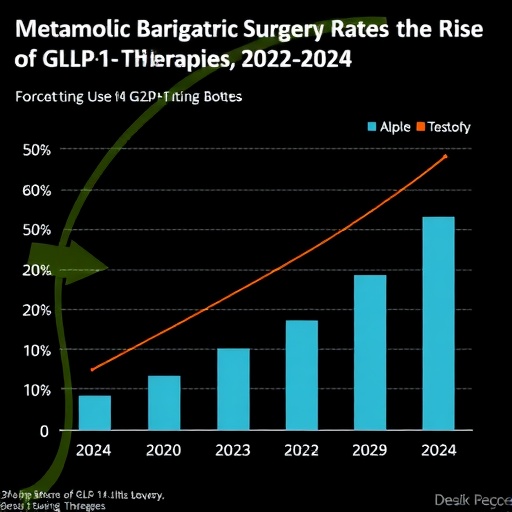
A recent investigative study published in JAMA Surgery has revealed significant shifts in the landscape of obesity treatment modalities, marking a pivotal moment in how metabolic health is managed clinically. Over a two-year period spanning from 2022 to 2024, the utilization of metabolic bariatric surgery witnessed a dramatic reduction by 34.1%, while the prescription and consumption of glucagon-like peptide-1 receptor agonists (GLP-1 RAs) surged by an astounding 140.4%. This divergent trend highlights a paradigm shift in therapeutic preferences, which may have profound implications for future healthcare approaches to obesity and related metabolic disorders.
Metabolic bariatric surgery, historically deemed the gold standard for sustained and effective weight reduction among patients with obesity, has long demonstrated remarkable efficacy not only in weight loss but also in the amelioration of associated metabolic comorbidities such as type 2 diabetes mellitus, hypertension, and dyslipidemia. Techniques such as Roux-en-Y gastric bypass and sleeve gastrectomy alter the anatomy and physiology of the gastrointestinal tract, leading to decreased caloric intake and alterations in gut hormone profiles. Despite its proven benefits, this study indicates a marked downturn in uptake likely influenced by the rising prominence and accessibility of pharmacological interventions.
The glucagon-like peptide-1 receptor agonists represent an innovative class of peptides that mimic endogenous incretin hormones, which are secreted by intestinal L-cells in response to nutrient ingestion. These pharmacotherapeutics enhance glucose-dependent insulin secretion, suppress glucagon release, and delay gastric emptying, thus contributing to appetite suppression and enhanced weight loss. The dramatic increase in GLP-1 RA utilization signals the medical community’s growing confidence in their safety profiles and efficacy, potentially shifting treatment paradigms away from invasive surgical procedures toward more patient-friendly pharmacotherapy.
Notably, the escalating prescription rates of GLP-1 receptor agonists may be attributed to several factors, including improved formulation, expanded indication approvals across various metabolic diseases, and increasing patient acceptance due to the non-invasive nature of the medication. Additionally, advances in molecular engineering have allowed for the development of longer-acting agents that provide sustained therapeutic effects with reduced dosing frequency, enhancing adherence and treatment outcomes.
Surgical intervention, albeit highly effective, is often accompanied by procedural risks, recovery times, and potential complications such as nutrient malabsorption, surgical site infections, or postoperative anatomical alterations. These challenges may deter some eligible patients from pursuing bariatric surgery. In contrast, GLP-1 receptor agonists offer a pharmacologic alternative that minimizes these concerns, providing a compelling treatment strategy especially for individuals with contraindications to surgery or those seeking less invasive options.
From a metabolic standpoint, the incretin-based therapies harness the body’s natural hormonal pathways to modulate energy balance and glucose homeostasis, attributes that are crucial in tackling the multifaceted pathophysiology of obesity. The confluence of improved patient outcomes and quality of life associated with GLP-1 receptor agonists underscores their potential to become central components in comprehensive metabolic health management programs.
The observed decline in bariatric surgical procedures concomitant with the rise in GLP-1 RA use may forecast an ongoing shift in clinical practice patterns. This trend reflects an evolving therapeutic landscape shaped by pharmaceutical innovation and patient-centered care models, which prioritize minimally invasive interventions with durable efficacy and manageable side effect profiles.
Medical professionals are now challenged to understand the long-term implications of this shift, especially in terms of sustained weight loss, metabolic improvement, and cost-effectiveness. While GLP-1 receptor agonists demonstrate promising short- and mid-term results, bariatric surgery remains unparalleled in achieving substantial and lasting weight reduction, posing important questions about patient selection criteria and treatment algorithms.
Moreover, the increasing reliance on pharmacotherapy necessitates vigilant monitoring for adverse effects, potential drug resistance, and adherence challenges, as well as considerations about equity of access given the typically high costs associated with these novel agents. Health systems must balance the benefits of emerging medical treatments with the well-established outcomes of surgical intervention to optimize comprehensive obesity care.
In parallel, ongoing clinical trials and research efforts are essential to delineate the comparative effectiveness of GLP-1 receptor agonists versus metabolic bariatric surgery across diverse patient populations. These investigations will also help clarify long-term safety profiles, mechanistic pathways, and potential synergies when combining surgical and pharmacological approaches.
As the prescribing of GLP-1 receptor agonists continues its upward trajectory, future healthcare models are likely to emphasize individualized treatment regimens that integrate pharmacology, lifestyle modification, and surgical options tailored to patient-specific metabolic and anatomical characteristics. This integrative strategy aims to maximize therapeutic efficacy while minimizing risks and enhancing patient satisfaction.
In summary, the study published in JAMA Surgery sheds light on a transformative period in obesity treatment, marked by a substantial reduction in metabolic bariatric surgeries alongside explosive growth in GLP-1 receptor agonist use. This dynamic is poised to reshape clinical decision-making, resource allocation, and ultimately patient outcomes in the domain of metabolic health and weight management.
Subject of Research: Trends in utilization of metabolic bariatric surgery and glucagon-like peptide-1 receptor agonists in obesity treatment
Article Title: Not specified
News Publication Date: Not specified
References: doi:10.1001/jamasurg.2026.1343
Keywords: Weight loss, Surgery, Metabolic health, Peptides, Agonists
Tags: comparison of bariatric surgery and GLP-1 therapiesdecline in bariatric surgery ratesefficacy of Roux-en-Y gastric bypassfutureGLP-1 receptor agonists weight loss effectsimpact of GLP-1 receptor agonists on obesity treatmentmetabolic bariatric surgery trends 2022-2024metabolic comorbidities and treatmentobesity management paradigm shiftrise of pharmacological obesity therapiessleeve gastrectomy outcomestype 2 diabetes and obesity interventions