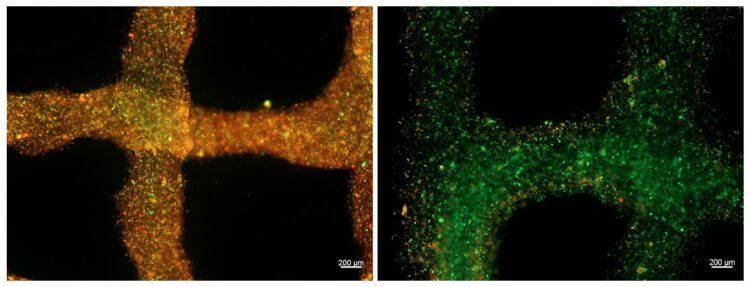
Newly developed bioink enhances the ability of implanted cells to grow and regenerate new tissue
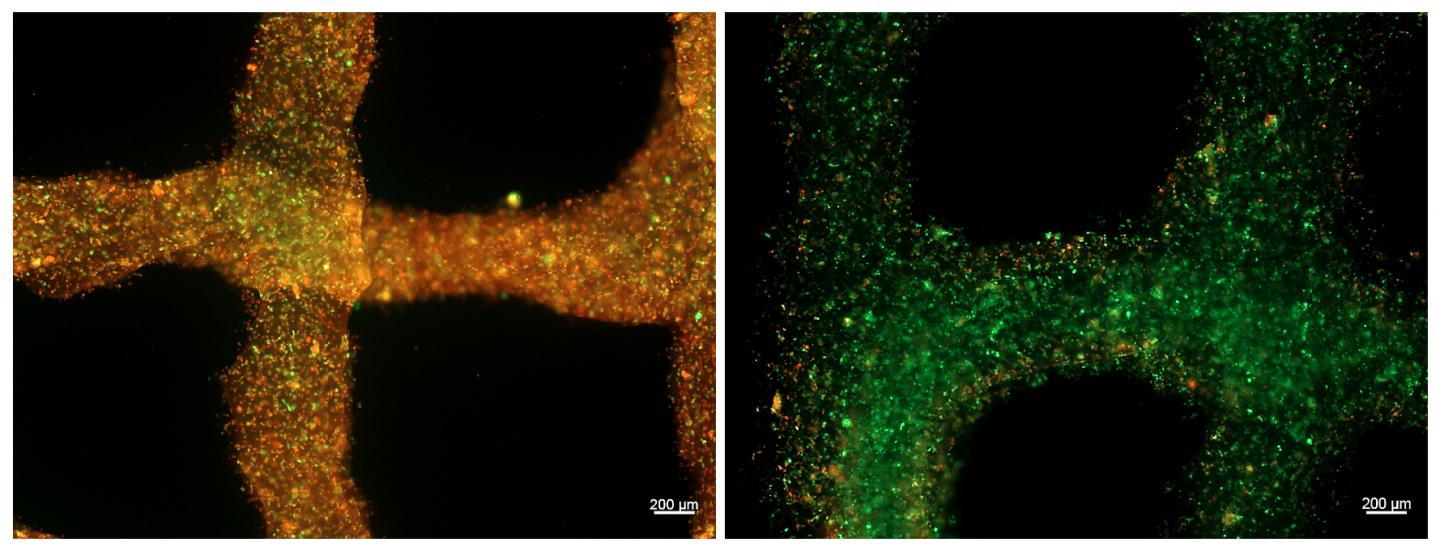
Credit: Khademhosseini Lab
(LOS ANGELES) – Engineering new tissues can be used to alleviate shortages of organs in transplantation, as well as to develop physiological models for drug discovery applications. One of the emerging approaches to building tissues is through 3D Printing, where cells and materials can be combined to make inks that can generate tissue structures. One of the limitations for making new tissues is that they require oxygen to survive. This oxygen is delivered through blood vessels, which take a few days to develop in a transplanted tissue.
A collaborative team, which includes a group from the Terasaki Institute for Biomedical Innovation (TIBI), has developed a bioink that offers a solution to this problem. This bioink can generate oxygen and deliver it to cells in 3D printed tissues to keep them alive before blood vessels penetrate the tissue. Therefore, when it is used in 3D bioprinting to construct tissue implants, the ability of cells to regenerate new tissue is greatly enhanced.
As discussed in their recent publication in Advanced Healthcare Materials, the TIBI group tested their oxygen-generating bioink extensively to optimize its chemical and physical properties. As a result, oxygen was delivered to the cells in the tissue constructs for the period necessary for blood vessels to develop fully. These blood vessels would then be able to resume their oxygen delivery functions, and the cells would have the additional support needed to grow and regenerate new tissue. The group also conducted separate experiments on tissue constructs using two different types of cells, including cardiac cells and muscle cells, and they demonstrated the positive effects of using the new bioink.
“By delivering oxygen to the implanted cells, we would be able to improve the tissue functionality and integration to the host tissue. A similar approach can be used to make functional tissues with improved survival for drug screening applications and pathophysiological studies within a long period of time,” said Samad Ahadian, Ph.D., lead investigator of the Terasaki Institute team.
Such developments can result in a variety of medical applications, including the enhancement of tissue regeneration in patients who have suffered a heart attack. These patients have experienced a period in which their heart is without a sufficient supply of oxygen. Therefore, there may be damage or a higher risk of harm to parts of their cardiac tissue. Tissue implants using the new bioink may help not only to increase the survival of the affected cardiac cells but can also help to support the growth and formation of the cardiac blood vessels.
###
Additional authors on the article include Ahmet Erdem, Mohammad Ali Darabi, Rohollah Nasiri, Sivakoti Sangabathuni, Yavuz Nuri Ertas, Halima Alem, Vahid Hosseini, Amir Shamloo, Ali S. Nasr, Mehmet R. Dokmeci, Ali Khademhosseini. Financial support came from the National Institutes of Health Foundation under grants 1R01EB021857 and R01GM126571 and the American Heart Association Transformational Project Award under grants 18TPA34230036 and TUBITAK-2219 (1059B191700093).
PRESS CONTACT
Stewart Han, [email protected], +1 818-836-4393
Terasaki Institute for Biomedical Innovation
The Terasaki Institute for Biomedical Innovation (terasaki.org) is a non-profit research organization that invents and fosters practical solutions that restore or enhance the health of individuals. Research at the Terasaki Institute leverages scientific advancements that enable an understanding of what makes each person unique, from the macroscale of human tissues down to the microscale of genes, to create technological solutions for some of the most pressing medical problems of our time. We use innovative technology platforms to study human disease on the level of individual patients by incorporating advanced computational and tissue-engineering methods. Our research teams translate findings yielded by these studies into tailored diagnostic and therapeutic approaches encompassing personalized materials, cells, and implants with unique potential and broad applicability to a variety of diseases, disorders, and injuries.
The Institute is made possible through an endowment from the late Dr. Paul I. Terasaki, a pioneer in the field of organ transplant technology.
Media Contact
Stewart Han
[email protected]
Original Source
https:/
Related Journal Article
http://dx.