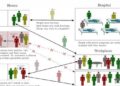
Credit: Florida Atlantic University
Measles was declared eradicated in the United States in 2000, but has reappeared in recent months in the form of outbreaks in several states. Of the 704 people in the U.S. infected with this highly contagious virus in 2019, 500 were never vaccinated and the remainder are likely to have never received a second follow up dose.
Outbreaks in New York City and Rockland County in New York, so far, seem to have emanated from ultra-Orthodox Jewish residents whose affected children were never vaccinated. In fact, the New York City Department of Health and Mental Hygiene has declared the measles outbreak affecting the ultra-Orthodox Jewish community in Williamsburg to be a public health emergency.
A specter of clinical, ethical, public health and legal concerns have been raised by these recent outbreaks, including the freedom of a parent to choose not to vaccinate. This decision should be viewed in the context of the need to achieve “herd immunity.” Herd immunity refers to the resistance to the spread of a contagious disease within a general population, which occurs only when a sufficiently high proportion of individuals are immune to the disease, especially through vaccination. The level of vaccination needed to achieve herd immunity for measles is 90 to 95 percent.
Researchers from Florida Atlantic University’s Schmidt College of Medicine have published a commentary in the American Journal of Medicine on these issues, motivated in part by the availability of important and relevant data from a small case series of interviews conducted with ultra-Orthodox Jewish mothers in Williamsburg and Rockland counties.
The available data include their perceived barriers to vaccinating their children. The failure to achieve herd immunity in Williamsburg and Rockland counties seems to have resulted from numerous factors. For example, some mothers regarded the practice with suspicion. In some circumstances, cultural rather than religious factors influenced the mothers’ decisions not to vaccinate. Some families chose not to vaccinate one or more children at all, and others favored a delayed vaccination schedule with longer breaks between vaccines. In addition, in some ultra-Orthodox neighborhoods, religious fatalism led to non-vaccination.
The increase in dissemination of anti-vaccination literature within ultra-Orthodox Jewish communities along with lack of trust in perceived agents of outside establishment present additional barriers to the success of externally-motivated health intervention and highlights the importance of outreach activities that seek to dispel suspicion and fear. In addition, families in ultra-Orthodox Jewish communities have an average of 8.33 children, which enhances the risk of disease transmission between children through co-mingling in close-quarters.
Poverty, limited secular education, large family size, and domestic over-crowding increase the vulnerability of ultra-Orthodox Jewish children to communicable disease outbreaks. Ultra-Orthodox Jewish households constitute 16 percent of the total New York City Jewish population, and more than 45 percent of these families live below 150 percent of the federal poverty line. Moreover, in 62 percent of these households neither parent has more than a high school diploma.
“Our data suggest the possibilities that establishing trust, influencing social networks as well as media and cultural or religious factors among ultra-Orthodox Jewish mothers may have a favorable impact on the measles vaccination,” said Charles H. Hennekens, M.D., Dr.P.H., senior author and the first Sir Richard Doll Professor and senior academic advisor in FAU’s Schmidt College of Medicine.
Hennekens and co-authors Rachael Silverberg, MPH, a rising third-year medical student; Jennifer Caceres, M.D., associate dean for student affairs; Sara Greene, MSW, coordinator, Department of Biomedical Science; all within FAU’s Schmidt College of Medicine; and Mark Hart, Ed.D., clinical assistant professor, University of Florida, note the possibilities that the strong influence of social networks among ultra-Orthodox Jewish families may be employed to combat the circulation of misinformation regarding vaccines.
“Community members of influence, including rabbis, health care practitioners, and mothers of high social standing should be identified and recruited to serve as advocates for childhood immunization,” said Silverberg. “The success of these partnerships would be dependent upon the strength and durability of relationships forged between health officials and the community.”
The authors also highlight other clinical challenges among the general U.S. population. Americans born between 1957 to 1989 have only received one dose of the measles, mumps and rubella (MMR) vaccine. Since 1989, two doses of the low-cost MMR vaccine is recommended because it confers 97 percent immunity from measles. Without vaccination, exposure to someone in the same room who has the disease confers a 90 percent chance of getting measles. Revaccination is indicated in patients who were vaccinated before their first birthday, received the killed measles vaccine (KMV), or were vaccinated between 1963 to 1967 with an unknown type of vaccine.
“Health care providers and their patients may wish to consider that vaccination of a few may abort future epidemics and the need for vaccination of many to reduce the preventable morbidity and mortality from measles,” said Hennekens.
###
About the Charles E. Schmidt College of Medicine:
FAU’s Charles E. Schmidt College of Medicine is one of approximately 152 accredited medical schools in the U.S. The college was launched in 2010, when the Florida Board of Governors made a landmark decision authorizing FAU to award the M.D. degree. After receiving approval from the Florida legislature and the governor, it became the 134th allopathic medical school in North America. With more than 70 full and part-time faculty and more than 1,300 affiliate faculty, the college matriculates 64 medical students each year and has been nationally recognized for its innovative curriculum. To further FAU’s commitment to increase much needed medical residency positions in Palm Beach County and to ensure that the region will continue to have an adequate and well-trained physician workforce, the FAU Charles E. Schmidt College of Medicine Consortium for Graduate Medical Education (GME) was formed in fall 2011 with five leading hospitals in Palm Beach County. In June 2014, FAU’s College of Medicine welcomed its inaugural class of 36 residents in its first University-sponsored residency in internal medicine and graduated its first class of internal medicine residents in 2017.
About Florida Atlantic University:
Florida Atlantic University, established in 1961, officially opened its doors in 1964 as the fifth public university in Florida. Today, the University, with an annual economic impact of $6.3 billion, serves more than 30,000 undergraduate and graduate students at sites throughout its six-county service region in southeast Florida. FAU’s world-class teaching and research faculty serves students through 10 colleges: the Dorothy F. Schmidt College of Arts and Letters, the College of Business, the College for Design and Social Inquiry, the College of Education, the College of Engineering and Computer Science, the Graduate College, the Harriet L. Wilkes Honors College, the Charles E. Schmidt College of Medicine, the Christine E. Lynn College of Nursing and the Charles E. Schmidt College of Science. FAU is ranked as a High Research Activity institution by the Carnegie Foundation for the Advancement of Teaching. The University is placing special focus on the rapid development of critical areas that form the basis of its strategic plan: Healthy aging, biotech, coastal and marine issues, neuroscience, regenerative medicine, informatics, lifespan and the environment. These areas provide opportunities for faculty and students to build upon FAU’s existing strengths in research and scholarship. For more information, visit fau.edu.
Media Contact
Gisele Galoustian
[email protected]