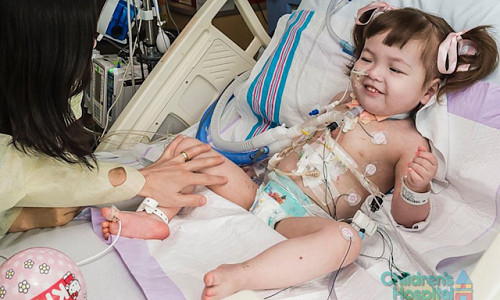
Only three months after she became the youngest person to receive a bioengineered organ, two-year-old Hannah Warren has died.
In an announcement posted online Monday, the Children’s Hospital of Illinois — where Hannah underwent a groundbreaking windpipe implant — confirmed the sad turn of events. “Although regenerative medicine remains in the early stages for pediatric patients, progress is being made,” the statement reads. “Hannah, and the physicians caring for her, helped advance this area of medical practice which is only at its very beginning stages.”
Doctors involved in the girl’s treatment told the New York Times that her death was not related to the bioengineered organ. Rather, her native tissue around the esophagus didn’t heal properly, necessitating another operation. She ultimately died from complications of that second operation. “The trachea was never a problem,” said Paolo Macchiarini, a surgeon at the Karolinska Institute in Stockholm, who led the girl’s tracheal implant and has spearheaded the protocol around the world.
The news got me thinking about a feature article I wrote two years ago about a similar procedure in which a toddler, about the same age as Hannah Warren, received a tissue-engineered blood vessel to correct a congenital heart defect known as a ‘single-ventricle anomaly’. The problem is fatal without surgical correction.
The bioengineered blood vessel, like the artificial trachea, starts out as a tube of plastic fibers. Doctors then add a patient’s own cells, taken from the bone marrow, and implant the construct after just a few hours of incubation. Twenty-five people received this treatment in Japan throughout the late 1990s and early 2000s, but this was the first such procedure in the US.
So how is that child doing today? “I am happy to report our first patient is still doing well nearly two years after her surgery,” Christopher Breuer told me in an email this week.
Breuer and his colleague Toshiharu Shinoka completed the operation in August 2011 at the Yale-New Haven Hospital in Connecticut. The two pediatric surgeons have since moved to Columbus, Ohio, where they codirect the Tissue Engineering Program at Nationwide Children’s Hospital. They continue to see their one patient from the blood vessel trial every six months and talk to her parents on the phone about once a month. But the move to Ohio has temporarily delayed further study enrollment.
They should be recruiting participants again soon, though. “We have recently completed construction of our new facilities,” says Breuer, “and will hopefully be enrolling more patients later this year.”
As for the bioengineered tracheas, Macchiarini told the Times that he would continue with similar operations, including one scheduled for Stockholm this week. It’s clear that with Hannah Warren’s death, the risks of the procedure will be foremost in researchers’ thoughts.
Story Source:
The above story is reprinted from materials provided by Nature, Elie Dolgin.