First evidence that repeated mass administration of ivermectin can reduce malaria incidence in children aged five or younger without an increase in adverse events for the wider population given the drug
First evidence that repeated mass administration of ivermectin can reduce malaria incidence in children aged five or younger without an increase in adverse events for the wider population given the drug.
Childhood malaria episodes could be reduced by 20% — from 2.49 to 2 cases per child — during malaria transmission season if the whole population were given a drug called ivermectin every three weeks, according to the first randomised trial of its kind including 2,700 people including 590 children from eight villages in Burkina Faso, published in The Lancet.
In addition, repeated mass administration of ivermectin showed no obvious drug-related harms among fellow villagers taking the drug.
Since 2000, deaths from malaria have dropped by 48% around the world and there are fewer endemic regions, but progress is stalling due to growing resistance to artemisinin; the drug that has been integral to that success.
Ivermectin is used to treat parasite infections from river blindness and scabies to head lice. It is regularly distributed in mass drug administrations for the control of neglected tropical diseases. Previous studies have shown it kills mosquitoes when they ingest ivermectin-treated human or animal blood, but none have looked at its effect on clinical malaria incidence.
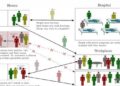
Study author, Dr Brian D Foy of Colorado State University, USA, says: “Ivermectin reduces new cases of malaria by making a person’s blood lethal to the mosquitoes who bite them, killing mosquitoes and therefore reducing the likelihood of infection of others. Because ivermectin has a unique mode of action compared to other malaria control insecticides and antimalarial drugs, it could be used alongside drugs that treat malaria to combat residual transmission of the disease.” [1]
The study authors set out to test the safety and efficacy of repeated mass ivermectin administration to control malaria during an 18-week trial during the 2015 rainy season. The research looked at children as they have the highest disease burden in hyperendemic communities because of their underdeveloped immunity. They invited eight villages to participate and four were assigned to each group. The intervention group had 1,447 participants including 327 children, and the control group 1,265 including 263 children.
All eligible residents — 1,080 in the intervention group and 999 in the control — received a single 150-200μg/kg dose of ivermectin plus 400mg of albendazole – an anti-worm medication. The intervention group received five further three-weekly doses of ivermectin alone, reaching 70-75% mass drug administration coverage. [2]
In the villages, children aged five or younger were tested for malaria every two weeks, and treated if needed. In the intervention group 648 malaria episodes occurred in 327 children, and the control group saw 647 among 263 children. Malaria episodes per child in the study villages were reduced by 20% in the intervention group compared to the control — from 2.49 to 2 cases per child — without any obvious drug-related harms to the population.
More than double the amount of children in the intervention group had no malaria episodes, compared with children in the control group: 20% [64/327 children] vs 9% [23/264 children].
Adverse reactions such as vomiting, pruritus, oedema in the limbs were recorded in 3% (45 out of 1,447) of the intervention group and 2% (24 out of 1,265) of the control group. There were similar levels of adverse reactions in the children (6% [18 of 327 children] in the intervention group and 5% [14 of 263 children] in the control group.
“Because of mosquitoes’ ability to adapt to control tools, new methods of preventing the transmission of malaria are needed, in particular those that target residual transmission. Ivermectin is well tolerated and widely used so it could be a useful tool in disease reduction if further trials show similar results.” Continues Dr Foy. [1]
The authors note that the villages selected had been studied previously and regularly treated with ivermectin and albendazole in the years before this study. In addition, their sample size is relatively small, and it was not possible to administer a placebo meaning participants and study teams knew who was and was not receiving treatment. The researchers aimed to mitigate this by assigning each nurse to work in one intervention group village and one control group village to control for nurse effects, and the field physician constantly monitored their work.
The researchers suggest there could be bias in the self-reporting of adverse events because villagers knew which group they were in. They note that there were more events reported in the intervention group, but none were drug related and very few were classified as serious adverse events.
These results are the first proof of principal of antimalarial effects of ivermectin and further work is required to test dosing and distribution approaches. The team call for further trials, in particular double-blinded trials from other endemic areas to test the drug against different malaria ecologies. Studies are also needed to examine the suspected direct antimalarial effects of repeated ivermectin treatment in infected humans. The authors also call for more safety studies in large populations.
Writing in a linked Comment, Dr N Regina Rabinovich of the Harvard T Chan School of Public Health, USA, says: “Foy and colleagues’ work is an important step for a promising, preventive intervention for malaria. The development of this new tool will require clear epidemiological (ie, human disease) impact and coordination with the neglected tropical diseases community, but the ultimate results could help us to get back on track to meet the global malaria goals.”
###
Peer-reviewed / Randomised controlled trial / People
NOTES TO EDITORS
This study was funded by Bill & Melinda Gates Foundation. It was conducted by researchers from Colorado State University, USA, Yale School of Public Health, USA, Institut de Recherche en Sciences de la Sante, Burkina Faso, Laboratoire Mixte International sur les Maladies à Vecteurs, Burkina Faso, University of Montpellier, France, Imperial College London, UK, Ministère de la Santé, Burkina Faso, Département de Recherche Clinique, Burkina Faso.
The labels have been added to this press release as part of a project run by the Academy of Medical Sciences seeking to improve the communication of evidence. For more information, please see: http://www.
[1] Quote direct from author and cannot be found in the text of the Article.
[2] Eligibility criteria were residence in the study village and consent after the trial was explained. Participants were excluded if they were less than 90cm tall, pregnant, breastfeeding an infant less than a week old, a history of travel to countries endemic with the filarial nematode Loa loa.
IF YOU WISH TO PROVIDE A LINK FOR YOUR READERS, PLEASE USE THE FOLLOWING, WHICH WILL GO LIVE AT THE TIME THE EMBARGO LIFTS: http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(18)32321-3/fulltext
Media Contact
Lancet Press Office
[email protected]
Related Journal Article
http://www.
http://dx.