Private insurance claim lines for STDs rose 76 % from 2007 to 2018
Credit: fairhealth.org
NEW YORK, NY–February 11, 2020–Private insurance claim lines for sexually transmitted diseases (STDs) rose 76 percent nationally from 2007 to 2018, according to a new study of STDs from FAIR Health, a national, independent nonprofit organization dedicated to bringing transparency to healthcare costs and health insurance information. The study results, which are being released today in the form of an infographic, are based on analysis of data from FAIR Health’s comprehensive repository of over 30 billion private healthcare claim records–the largest in the country.
According to the Centers for Disease Control and Prevention (CDC), combined cases of syphilis, gonorrhea and chlamydia, the three most commonly reported STDs, reached an all-time high in the United States in 2018. FAIR Health’s findings shed new light on this growing public health issue.
Among the results of the FAIR Health study:
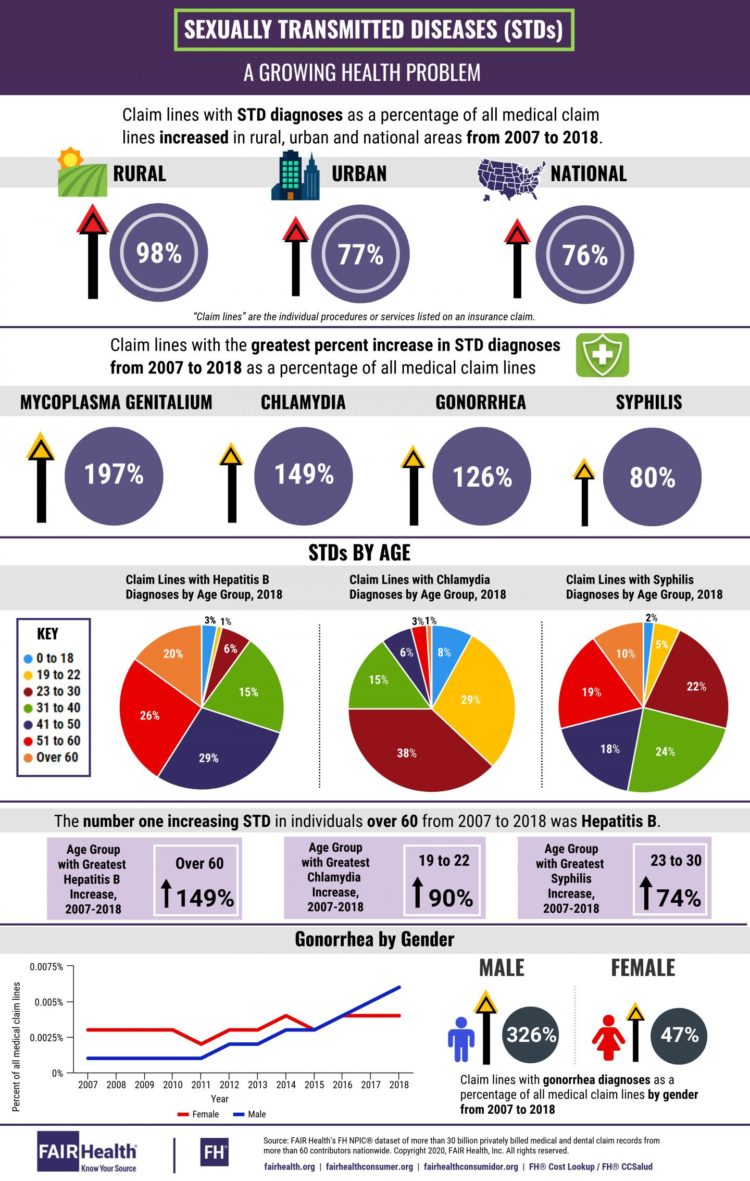
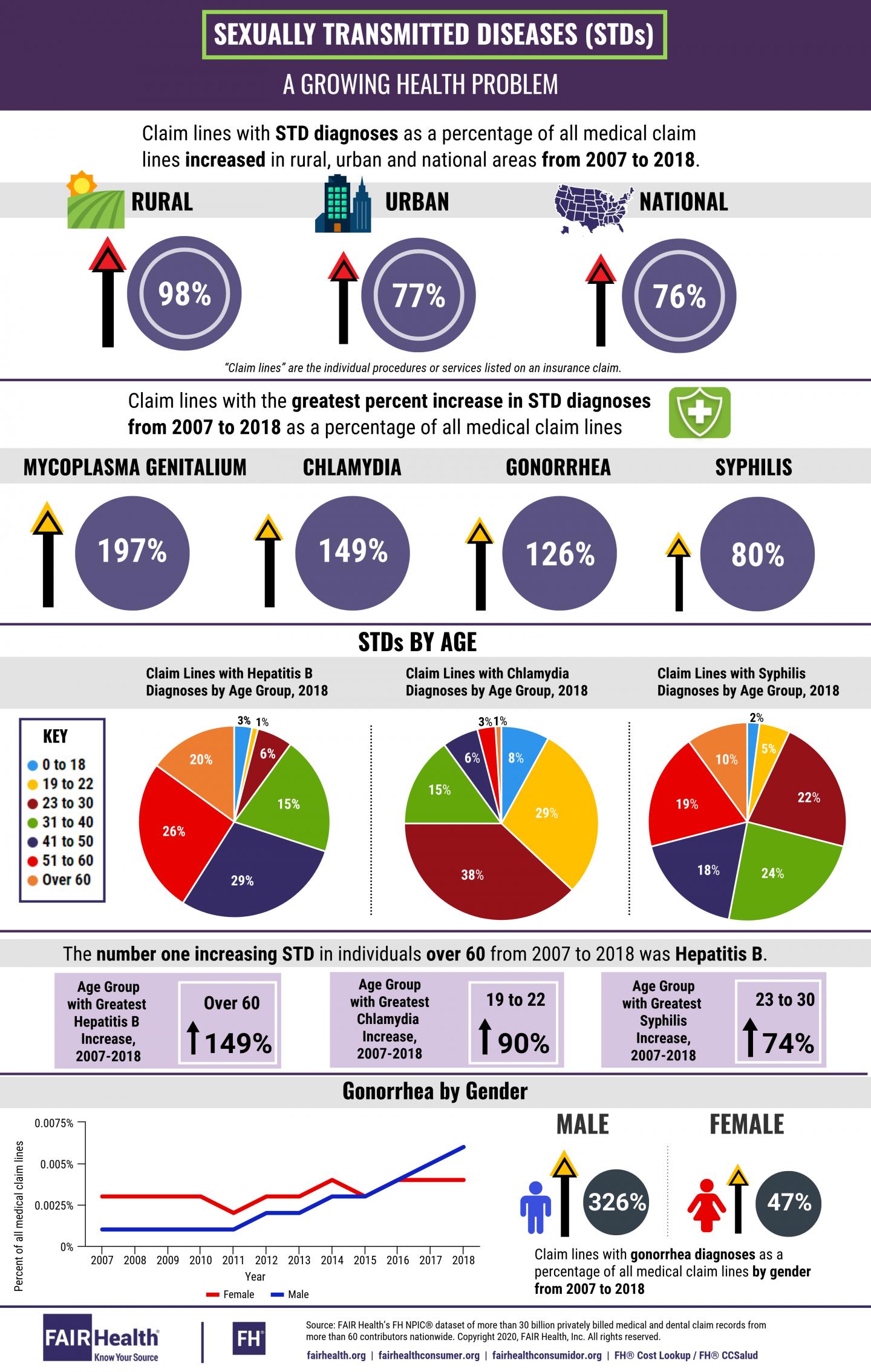
- Claim lines with STD diagnoses, as a percentage of all medical claim lines, increased nationally 76 percent from 2007 to 2018, but the increase was even greater in rural areas–98 percent, compared to 77 percent in urban areas.
- The four STD diagnoses whose associated claim lines had the greatest percent increase from 2007 to 2018 as a percentage of all medical claim lines were:
- Mycoplasma genitalium (MG or Mgen)–increased 197 percent;
- Chlamydia–increased 149 percent;
- Gonorrhea–increased 126 percent; and
- Syphilis–increased 80 percent.
- The age groups most associated with STDs in 2018 varied by the specific disease. The age groups that accounted for the largest share of claim lines were:
- Age 41-50 for hepatitis B (29 percent);
- Age 23-30 for chlamydia (38 percent); and
- Age 31-40 for syphilis (24 percent).
- From 2007 to 2018, claim lines with gonorrhea diagnoses as a percentage of all medical claim lines by gender increased 326 percent in males compared to 47 percent in females.
- In individuals over age 60, hepatitis B was the STD that showed the highest percent increase in claim lines from 2007 to 2018, and claim lines for hepatitis B increased more in the over 60 cohort (149 percent) than in any other age group.
- The age groups with the greatest increase in claim lines from 2007 to 2018 were:
- Age 19-22 for chlamydia (90 percent); and
- Age 23-30 for syphilis (74 percent).
FAIR Health President Robin Gelburd stated: “It is central to FAIR Health’s mission to use our vast repository of claims data to research public health concerns and support such research by others. We hope this information brings greater clarity to the growing problem of STDs.”
###
For the FAIR Health infographic on STDs, click here.
Follow us on Twitter @FAIRHealth
About FAIR Health
FAIR Health is a national, independent nonprofit organization dedicated to bringing transparency to healthcare costs and health insurance information through data products, consumer resources and health systems research support. FAIR Health possesses the nation’s largest collection of private healthcare claims data, which includes over 30 billion claim records contributed by payors and administrators who insure or process claims for private insurance plans covering more than 150 million individuals. FAIR Health licenses its privately billed data and data products–including benchmark modules, data visualizations, custom analytics and market indices–to commercial insurers and self-insurers, employers, providers, hospitals and healthcare systems, government agencies, researchers and others. Certified by the Centers for Medicare & Medicaid Services (CMS) as a national Qualified Entity, FAIR Health also receives data representing the experience of all individuals enrolled in traditional Medicare Parts A, B and D; FAIR Health houses data on Medicare Advantage enrollees in its private claims data repository. FAIR Health can produce insightful analytic reports and data products based on combined Medicare and commercial claims data for government, providers, payors and other authorized users. FAIR Health’s systems for processing and storing protected health information have earned HITRUST CSF certification and achieved AICPA SOC 2 compliance by meeting the rigorous data security requirements of these standards. As a testament to the reliability and objectivity of FAIR Health data, the data have been incorporated in statutes and regulations around the country and designated as the official, neutral data source for a variety of state health programs, including workers’ compensation and personal injury protection (PIP) programs. FAIR Health data serve as an official reference point in support of certain state balance billing laws that protect consumers against bills for surprise out-of-network and emergency services. FAIR Health also uses its database to power a free consumer website available in English and Spanish and an English/Spanish mobile app, which enable consumers to estimate and plan for their healthcare expenditures and offer a rich educational platform on health insurance. The website has been honored by the White House Summit on Smart Disclosure, the Agency for Healthcare Research and Quality (AHRQ), URAC, the eHealthcare Leadership Awards, appPicker, Employee Benefit News and Kiplinger’s Personal Finance. FAIR Health also is named a top resource for patients in Dr. Marty Makary’s book The Price We Pay: What Broke American Health Care–and How to Fix It and Elisabeth Rosenthal’s book An American Sickness: How Healthcare Became Big Business and How You Can Take It Back. For more information on FAIR Health, visit fairhealth.org.
Media Contact
Dean Sicoli
[email protected]
646-664-1645
Original Source
https:/