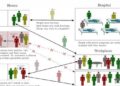
1. Screening all donated blood for Zika virus is not cost-effective in the United States
Abstract: http://annals.
Editorial: http://annals.
URLs go live when the embargo lifts
Universal screening of individual blood donations for Zika virus, which began in 2016, was not cost-effective in the 50 states during the first year. Widespread screening would only be cost-effective in the high mosquito season in Puerto Rico and never in the 50 states. Findings from a microsimulation study are published in Annals of Internal Medicine.
The Zika epidemic of the Americas beginning in 2015 is the largest outbreak to date. Because Zika virus is associated with severe illness, such as Guillain-Barre syndrome, and potentially devastating birth defects, such as microcephaly, the U.S. Food and Drug Administration (FDA) implemented measures to protect transfusion recipients from infection. In 2016, the FDA began requiring universal individual donation nucleic acid testing (ID-NAT) of donated blood for Zika virus in U.S. states and territories. Universal screening is still required today, although mini-pool NAT (MP-NAT) is permitted as of July 2018. However, the effectiveness and cost-effectiveness of these measures had not been evaluated previously.
Researchers from Stanford University, Vitalant Research Institute, and the American Red Cross used a microsimulation to estimate the effectiveness and cost-effectiveness of universal ID-NAT, universal mini-pool NAT, and alternative Zika virus screening policies in Puerto Rico and the 50 states. The microsimulation captured Zika-related harms to transfusion recipients, sexual partners, and their infants to weight the cost/benefit of universal screening. They found that during the first year of testing, screening was cost-effective only in the high mosquito season in Puerto Rico, and no evaluated screening policy was cost-effective in the 50 states. Because the Zika epidemic is largely over, screening policies are much less cost-effective today than during the period of their analysis. These findings suggest that revisiting the universal blood screening policy would be warranted. However, the authors note that many other considerations should inform blood safety policies in addition to cost-effectiveness.
Media contact: For an embargoed PDF, please contact Lauren Evans at [email protected]. To interview the first author, W. Alton Russell, MS, or the senior author, Brian Custer, PhD, please contact Courtney Griggs (Vitalant) at [email protected] or (480) 675-5754. The media team at the American Red Cross can be reached at [email protected] or (202) 303-5551.
2. Students deliberately infected by parasite shed light on cause of Katayama syndrome
Abstract: http://annals.
URLs go live when the embargo lifts
Katayama syndrome can occur in the absence of parasite eggs, suggesting that newly expressed antigens on developing worms may be the cause of illness. Understanding the cause of this syndrome can aid in identifying an appropriate treatment. A brief case report of students deliberately infected by schistosoma larvae is published in Annals of Internal Medicine.
Katayama syndrome is a self-limited illness that occurs several weeks after infection with Schistosoma larvae. Symptoms may become severe or lead to chronic illness, so it is important to understand the root cause.
Two human participants were infected with male cercariae of Schistosoma mansoni by researchers from Leiden University Medical Center. Only male parasitic worms were used so that they could not produce eggs in their hosts. Both participants developed Katayama syndrome, as evidenced by typical illnesses at the expected time after exposure, even in the absence of eggs. Based on an observation of the two participants, the researchers concluded that Katayama syndrome can present with remarkable heterogeneity in clinical signs and symptoms and may be nonspecific enough to make diagnosis difficult. According to the authors, the cases show that eosinophillia and seroconversion may become apparent after severe symptoms have subsided, that Katayama syndrome can be diagnosed as early as 5 weeks after exposure, and that it is not necessarily related to egg deposition.
Media contact: For an embargoed PDF, please contact Lauren Evans at [email protected]. To interview the lead authors, please contact Sietzke Vermeulen at [email protected].
Special Section:
3. Annals readers share their perspectives on prescribing and recommending marijuana
Six commentaries were selected from among 100 submissions on topics ranging from marijuana policy to marijuana use during pregnancy
Recently, the editors of Annals of Internal Medicine asked readers to share their perspectives on prescribing or recommending marijuana. From 100 submissions, the editors chose to publish six essays that touched on some of the most important issues that clinicians face when discussing marijuana with their patients. Commentaries featured include:
- Cannabinoid Dosing for Chronic Pain Management
- Advocating for Blunt Policy
- Treating Pain: The Cannabis Conundrum
- Marijuana Use During Gestation and Lactation: Harmful Until Proved Safe
- Marijuana and Cardiovascular Disease: What Should We Tell Patients?
- Adverse Effects of Medical Marijuana: Observations from the Emergency Department
Media contact: For an embargoed PDF or author contact information for any or all of the articles, please contact Lauren Evans at [email protected].
###
Also New in this issue:
Beyond Pharmacotherapy: Lifestyle Counseling Guidance Needed for Hypertension
E. Amy Janke, PhD; Caroline Richardson, MD; Kristin L. Schneider, PhD
Ideas and Opinions
Abstract: http://annals.
Service Guarantees Have a Place in Health Care
Leonard L. Berry, PhD, MBA
Ideas and Opinions
Abstract: http://annals.
Private Equity Acquisition of Physician Practices
Lawrence P. Casalino, MD, PhD; Rayhan Saiani, MD; Sami Bhidya, MS; Dhruv Khullar, MD, MPP; Eloise O’Donnell, MPH
Abstract: http://annals.
Media Contact
Lauren Evans
[email protected]
215-351-2513