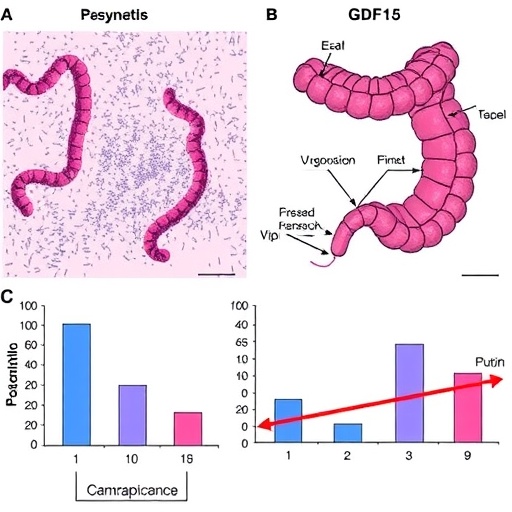
Emerging research from a team led by Hashimoto et al. sheds light on a significant hurdle in colorectal cancer treatment—chemoresistance. Their groundbreaking study, recently published in the British Journal of Cancer, explores how the protein Growth Differentiation Factor 15 (GDF15) plays a central role in promoting resistance against two frontline chemotherapeutic agents, 5-Fluorouracil (5-FU) and Oxaliplatin. This discovery highlights a previously underappreciated mechanism whereby colorectal cancer cells adopt stem cell-like traits, thus intensifying their ability to evade therapeutic assaults and sustain tumor growth.
Colorectal cancer remains one of the most prevalent and lethal malignancies worldwide, with chemotherapy standing as a cornerstone of management across various disease stages. Despite advances in therapeutic regimens, drug resistance continues to compromise patient outcomes, frequently leading to relapse and metastasis. The study by Hashimoto and colleagues pioneers in connecting GDF15, a cytokine widely recognized for its diverse roles in inflammation and metabolism, to the acquisition of a stem cell-like phenotype that underpins chemoresistance in colorectal cancer.
Cancer stem cells (CSCs) represent a subpopulation within tumors characterized by their capacity for self-renewal, differentiation, and inherent resilience against chemotherapeutic drugs. These cells are often blamed for tumor relapse and metastatic spread, making the identification of factors driving CSC properties a critical research area. The current study employs sophisticated in vitro and in vivo methods to demonstrate that elevated levels of GDF15 correlate strongly with increased CSC markers and heightened resistance to both 5-FU and Oxaliplatin.
Mechanistically, GDF15 appears to orchestrate a complex signaling cascade that reprograms colorectal cancer cells toward a stem cell-like state. This process involves modulation of various pathways such as Wnt/β-catenin and Notch signaling, both well-established regulators of stemness. By enhancing these pathways, GDF15 facilitates not only survival under chemotherapeutic stress but also promotes cellular plasticity allowing for tumor heterogeneity, a hallmark of aggressive cancers.
The investigators meticulously quantified GDF15 expression across multiple colorectal cancer cell lines and patient-derived tumor samples, observing a consistent pattern where higher GDF15 levels coincided with reduced sensitivity to chemotherapy. Functional assays further revealed that silencing GDF15 restored drug responsiveness and diminished CSC characteristics, underscoring its potential as a therapeutic target. These insights, if translated clinically, could revolutionize strategies to overcome chemoresistance in colorectal cancer.
Moreover, the research delves into the potential therapeutic implications of targeting GDF15. By inhibiting GDF15 signaling, either through monoclonal antibodies or small molecule inhibitors, it may be possible to sensitize resistant tumor cells to 5-FU and Oxaliplatin. This dual approach—disrupting the cancer stem cell niche while administering conventional chemotherapy—could ultimately reduce relapse rates and improve long-term survival outcomes for patients.
Importantly, the article emphasizes the heterogeneity of colorectal tumors and the intricacies of tumor microenvironment interactions. GDF15’s role is not limited to intrinsic tumor cell properties but extends to modulating immune responses and stromal cell behavior. This multifaceted impact suggests that therapeutic strategies targeting GDF15 might also enhance anti-cancer immunity, potentially synergizing with emerging immunotherapies.
Scientists used advanced transcriptomic profiling to identify downstream gene expression changes induced by GDF15. Results highlighted a shift towards genes that favor epithelial-mesenchymal transition (EMT), motility, and invasiveness—all characteristics that confer metastatic potential alongside chemoresistance. This reaffirms the link between stemness and aggressive disease phenotypes, further highlighting the importance of GDF15 as a node integrating these malignant features.
The clinical relevance of this study is reinforced by correlating patient survival data with GDF15 expression levels. Patients exhibiting high GDF15 tumor expression showed markedly poorer responses to standard chemotherapy and worse overall prognosis. This correlation paves the way for developing GDF15 as a prognostic biomarker, enabling clinicians to stratify patients and personalize treatment regimens accordingly.
In addition to therapeutic considerations, this research provides crucial insights into colorectal cancer biology. It encourages a paradigm shift from solely targeting proliferating tumor cells toward addressing the root cause of tumor persistence and recurrence—the cancer stem cell compartment. By unraveling the molecular players such as GDF15 that fuel this compartment, researchers are opening new avenues for durable cancer control.
The study also raises important questions regarding the regulation of GDF15 itself. Understanding upstream signals that trigger GDF15 expression in colorectal cancer could identify further targets for intervention. For instance, stress-induced factors in the tumor microenvironment or epigenetic modifications might be responsible for its aberrant overexpression, offering additional layers of potential therapeutic targeting.
Overall, the evidence presented positions GDF15 as a linchpin in colorectal cancer’s resistance machinery, linking stem-like phenotypic plasticity with escape from chemotherapeutic elimination. This discovery could catalyze the development of novel combination therapies where targeting GDF15 enhances the efficacy of existing drugs, ultimately improving patient survival and quality of life.
Moving forward, clinical trials designed to inhibit GDF15 signaling in tandem with standard chemotherapy will be critical to validate these findings in patient cohorts. Such trials would also shed light on potential side effects and the broader systemic roles of GDF15, informing safe and effective therapeutic designs. The promise of GDF15 as both a biomarker and a therapeutic target places it at the forefront of colorectal cancer research.
In summary, Hashimoto and colleagues have unraveled a crucial mechanism by which colorectal cancer cells evade chemotherapy. By promoting a stem cell-like phenotype through GDF15 upregulation, these cancer cells gain a formidable ability to resist 5-Fluorouracil and Oxaliplatin. This landmark study not only enhances our comprehension of cancer stem cell biology but also offers tangible clinical pathways to surmount one of oncology’s most vexing challenges: chemoresistance.
As the oncology community continues to grapple with improving outcomes for colorectal cancer, targeting GDF15 represents a beacon of hope. Integrating these insights into clinical practice could mark a transformative leap, refashioning colorectal cancer therapy from reactive treatment to precise molecular intervention. The intersection of stem cell dynamics, tumor microenvironment, and drug resistance exemplified by GDF15 promises an exciting frontier in cancer medicine.
Subject of Research: The role of Growth Differentiation Factor 15 (GDF15) in promoting resistance to chemotherapy (5-Fluorouracil and Oxaliplatin) by fostering a stem cell-like phenotype in colorectal cancer.
Article Title: GDF15 promotes 5-Fluorouracil and Oxaliplatin resistance by promoting stem cell-like phenotype in colorectal cancer.
Article References:
Hashimoto, M., Urabe, S., Hata, T. et al. GDF15 promotes 5-Fluorouracil and Oxaliplatin resistance by promoting stem cell-like phenotype in colorectal cancer. Br J Cancer (2026). https://doi.org/10.1038/s41416-026-03379-0
Image Credits: AI Generated
DOI: 12 May 2026
Tags: 5-Fluorouracil resistance mechanismscancer stem cell-like traits in chemoresistancecancer stem cells and tumor relapsecolorectal cancer drug resistance pathwaysGDF15 and colorectal cancer chemoresistanceGrowth Differentiation Factor 15 in cancerimpact of cytokines on cancer therapyinflammation-relatedmechanisms of chemotherapy evasion in colorectal cancerOxaliplatin resistance in colorectal cancerrole of GDF15 in chemotherapy resistancetherapeutic targets for chemoresistant colorectal tumors