American Journal of Preventive Medicine focus on critical public health aspects of COVID-19
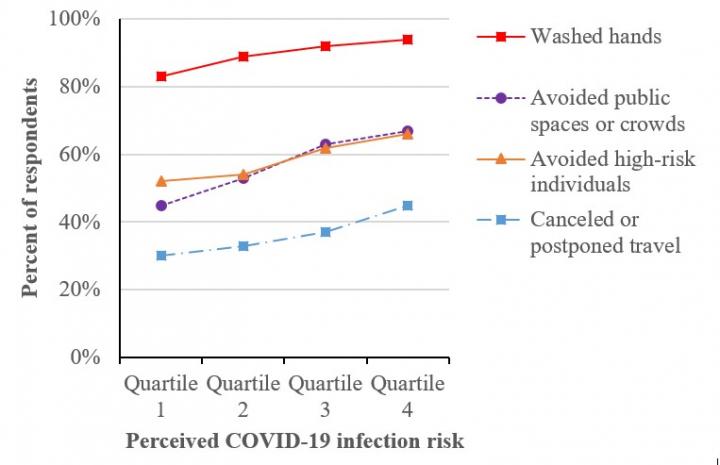
Credit: American Journal of Preventive Medicine
Ann Arbor, July 13, 2020 — New research and guidance in the American Journal of Preventive Medicine, published by Elsevier, focus on critical topics pertaining to community and individual health during the COVID-19 epidemic.
Researchers issue a transdisciplinary “Call to Action” to strengthen pandemic behavioral science to overcome COVID-19
The only evidence-based strategy currently available to halt the transmission of COVID-19 is population-wide behavior change. Although information about COVID-19 protective behaviors such as hand washing, mask wearing, and social distancing has been widely disseminated in the United States by federal and local governments, research has shown significant gaps in the public’s understanding and behavior, maybe because of inconsistency and lack of optimal tailoring. Researchers say the narrative is missing the behavioral science expertise that is central to achieving protective behaviors. “Fighting this pandemic will require new ‘weapons’ and a new resolve on the part of the government and the public,” says lead author John Allegrante, PhD, Columbia University’s Teachers College and the Mailman School of Public Health, New York, NY, USA. “A national historic commitment is needed in which behavior change methodology is a dominant weapon in the nation’s public health arsenal.” The researchers say there is an urgent need for accurate data about the public understanding of COVID-19 risk and preferred sources for obtaining information about how to stay safe. Better utilization of digital technology would enable more efficient targeting of at-risk individuals and tailoring of behavioral interventions. And, to drive these changes now and for the future, pandemic behavioral science, methodology, and evidence need to be updated and expanded.
“Preventing COVID-19 and Its Sequela: “There is No Magic Bullet . . . It’s Just Behaviors,” by John P. Allegrante, PhD, M. Elaine Auld, MPH, and Sundar Natarajan, MD, MSc (https:/
Perception of the risk of contracting or dying from COVID-19 strongly influences people’s decision to take protective actions, a national survey finds
As coronavirus began to spread across the United States, researchers conducted a cross-sectional national online survey between March 10 and March 31, 2020 asking participants to assess their risk of COVID-19 infection and fatality. They were also asked about behaviors they had taken to protect themselves from infection such as washing hands or avoiding public spaces and crowds. Individuals disagreed about the risks, and those perceiving higher risk were significantly more likely to engage in protective actions. Risk perceptions for getting COVID-19 and people’s willingness to act upon them grew stronger in responses provided after March 13, 2020, when many states declared school closures and bans on large gatherings, and the US declared a state of emergency and implemented travel bans. “Our findings suggest that to motivate protective actions, clear and consistent risk messages are needed. This was the case when states were closing down in March 2020. It will likely also be important when states open up again,” observes lead investigator Wändi Bruine de Bruin, PhD, Sol Price School of Public Policy, Dornsife Department of Psychology, Schaeffer Center for Health Policy and Economics; and Center for Economic and Social Research, University of Southern California, Los Angeles, CA, USA.
“Relationships Between Initial COVID-19 Risk Perceptions and Protective Health Behaviors: A National Survey,” by Wändi Bruine de Bruin, PhD, and Daniel Bennett, PhD (https:/
Financial strain associated with COVID-19 hospitalization may be felt most by younger patients with lower premium, higher deductible health plans
Out-of-pocket spending associated with hospitalizations for respiratory conditions similar to those caused by COVID-19 from January 2016 through August 2019 were significantly higher for patients who have a consumer-directed health plan (CDHP) that features lower premiums but higher deductibles compared with patients who had a traditional, low deductible plan. The difference was largest for those under 21 years old, and decreased as age increased. The largest increase was in the first half of the year when, the researchers note, younger people have likely not exceeded their deductibles. Although some insurers are waiving cost-sharing payments for a hospitalization related to COVID-19, self-insured employers are exempt. “Congress is now debating whether or not to require all plans to waive cost sharing related to COVID-19 treatment. Our findings suggest they might want to take action on cost-sharing waivers, because those out-of-pockets costs are otherwise going to be high for many people,” says lead investigator Matthew Eisenberg, PhD, Department of Health Policy and Management, Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA.
“Financial Risk for COVID-19 Respiratory Hospitalizations in Consumer-Directed Health Plans,” by Matthew D. Eisenberg, PhD, Colleen L. Barry, PhD, MPP, Cameron Schilling, MPH, and Alene Kennedy-Hendricks, PhD (https:/
Researchers warn that a lack of a racial/ethnic identifier in health records and medical data may lead to worse health outcomes for Arab Americans during the COVID-19 crisis and beyond
There are increasing calls to better understand the inequities populations of color face in the United States with regard to COVID-19, including increased infection rates, more severe disease, and greater risk of death. Potential health disparities for Arab Americans may never be recognized, however, because most medical data and surveys do not include an option to identify as Arab American. Author Nadia N. Abuelezam, ScD, Boston College William F. Connell School of Nursing, Chestnut Hill, MA, USA, observes that Arab Americans are asked to identify as non-Hispanic white, despite the fact that their health outcomes are significantly different. Arab Americans may be at increased risk for COVID-19 due to xenophobia and stigma, pre-existing conditions, crowded living conditions, lack of social support for new immigrants, and poor adoption of prevention behavior. “Arab Americans have long been ‘invisible’ in the medical and public health literature due to a lack of an ethnic identifier,” explains Dr. Abuelezam. “The COVID-19 crisis has forced the medical and public health community to reimagine the ways that healthcare can be provided and data can be collected in real time. In this moment of reimagination and creativity, we can embrace and enhance our racial and ethnic reporting measures to ensure we are collecting data on all ethnic and racial subgroups in the US.”
“Health Equity During COVID-19: The Case of Arab Americans,” by Nadia Abuelezam (https:/
###
Media Contact
Jillian B. Morgan
[email protected]
Original Source
https:/
Related Journal Article
http://dx.