Treatment option for hypereosinophilic syndrome, a group of rare blood disorders, OK’d by FDA
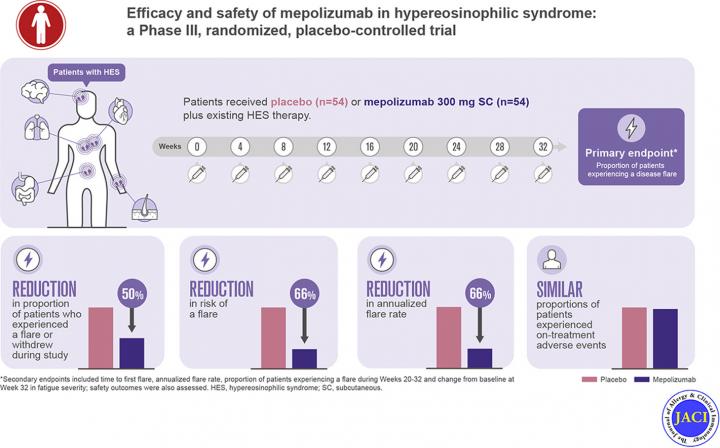
Credit: Journal of Allergy and Clinical Immunology
Following two decades of research on a group of rare diseases called hypereosinophilic syndrome at Cincinnati Children’s Hospital Medical Center, the U.S. Food and Drug Administration has approved the drug Nucala (mepolizumab) for use in the treatment of patients with hypereosinophilic syndrome.
Hypereosinophilic syndrome, also known as HES, is a life-threatening group of blood disorders that involve having high levels of eosinophils, a type of white blood cell that plays an important role in the immune system. Over time, these overly high levels of eosinophils enter tissues and organs and cause damage. Until now, high doses of corticosteroids were used to lower eosinophil levels to prevent damage to organs. However, disease flares still happen, and these disease flares cause dangerous damage to the body.
The FDA stated in a Sept. 25 news release that the agency had approved Nucala (mepolizumab) for patients 12 or older with HES for six months or longer without another identifiable non-blood related cause of the disease.
“We at Cincinnati Children’s scored a home run in that we have been pursuing this for two decades on behalf of patients through our research,” said Marc Rothenberg, MD, PhD, director of the Division of Allergy and Immunology and the Cincinnati Center for Eosinophilic Disorders at Cincinnati Children’s.
“We specialize in eosinophilic disorders, and this is a big breakthrough for the patients,” added Rothenberg, who was involved in related translational research and the clinical trials of mepolizumab that preceded FDA approval. “People with rare diseases have to really fight for improved treatments and their on-label approval, and it’s a long journey.”
Mepolizumab, a biological antibody that blocks the eosinophil growth factor IL-5, was approved as an asthma drug in 2015.
FDA approval to treat hypereosinophilic syndrome means “that patients with HES have a treatment option that will reduce their disease flares and have improved health, without substantial side effects of this medicine,” Rothenberg said.
Rothenberg focuses his lab’s research on elucidating the mechanisms of allergic responses, especially in mucosal tissues such as the gastrointestinal tract and lung.
Support for Rothenberg’s research has included funding from the Campaign Urging Research for Eosinophilic Diseases (CURED), which welcomed news of FDA approval for the new use of mepolizumab.
“This decision means so much to patients and their families,” said Ellyn Kodroff, founder and director of the Campaign Urging Research for Eosinophilic Diseases. “Having FDA approval allows patients to afford this drug with insurance coverage, giving hope for a better and longer life. CURED is so proud to have raised and donated millions of dollars funding translational research underlying the rationale for targeting interleukins for eosinophilic conditions, like mepolizumab does. This continuing research supporting unmet needs for rare eosinophilic diseases is life changing.”
Rothenberg began researching eosinophils as a doctoral student at Harvard University in the 1990s. It was at that time that he showed involvement of IL-5 in human disease and its effects on eosinophils.
At Cincinnati Children’s, Rothenberg, along with other researchers around the world, provided evidence that eosinophils were pro-inflammatory cells involved in allergic diseases. Rothenberg and his colleagues contributed to the rationale of targeting eosinophils, including performing clinical studies in patients with a variety of eosinophilic disorders.
In 2008, Rothenberg led an international group of investigators to conduct a randomized clinical trial that proved the ability of mepolizumab to lower oral steroid doses in patients with HES (Rothenberg et al. New England Journal of Medicine 2008 Mar 20;358(12):1215-28. doi: 10.1056/NEJMoa070812. Epub 2008 Mar 16. PMID: 18344568).
Despite meeting the primary endpoint of the study, the FDA tightened its criteria for approval of mepolizumab, Rothenberg said. It took an additional decade of research to eventually meet the FDA’s requested endpoints, focused on the clinical benefit of mepolizumab in this rare disease population.
As described in a recent publication in the Journal of Allergy and Clinical Immunology of the results of the phase 3, randomized, placebo-controlled trial in adolescent and adult patients with HES investigating the efficacy and safety of mepolizumab, mepolizumab was shown to reduce the number of HES disease flares (Roufesse et al. Journal of Allergy and Clinical Immunology 2020 Sep 18; S0091-6749(20)31276-8. doi: 10.1016/j.jaci.2020.08.037.). The 108 patients in the trial were from 39 centers and 13 countries.
###
The clinical trial was supported by GlaxoSmithKline. Underlying research in the Rothenberg CURED Laboratory was supported by the National Institutes of Health, Campaign Urging Research for Eosinophilic Diseases (CURED), Sunshine Charitable Foundation and its supporters Denise and David Bunning.
Media Contact
Barrett J. Brunsman
[email protected]
Related Journal Article
http://dx.