In a landmark study published on April 22, 2026, researchers have shed significant light on a contentious surgical debate pivotal for hepatocellular carcinoma (HCC) treatment. The study, featured in the British Journal of Cancer, unpacks the comparative efficacy of two major surgical techniques employed during laparoscopic major hepatectomy (LMH): the Glissonian approach versus the hilar dissection approach. This randomized controlled trial stands as the first of its kind to systematically evaluate both short- and long-term outcomes of these distinctive methods in patients undergoing surgery for HCC.
Laparoscopic major hepatectomy has revolutionized liver surgery by enabling minimally invasive removal of significant hepatic tissue with reduced morbidity. However, the operative management of the hepatic hilum—the region encompassing the portal vein, hepatic artery, and bile duct—remains a formidable challenge. The optimal technique to control this complex anatomical area during LMH has been a subject of debate, with surgeons divided on which approach confers greater safety and efficacy.
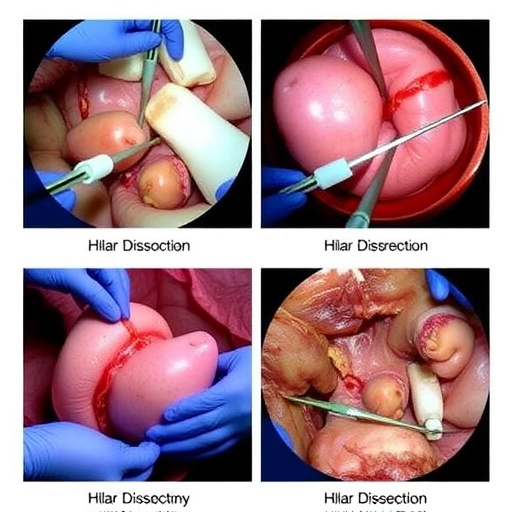
The Glissonian approach centers on the en bloc extrahepatic control of the Glissonian sheath, a connective tissue sheath that envelops the portal triad structures. This technique theoretically allows for simultaneous vascular and biliary pedicle control, leading to potentially faster and less blood loss-prone surgery. Conversely, the hilar dissection technique involves meticulous individual dissection and ligation of each portal structure, providing precise anatomical clearance but often prolonging operative time and increasing the risk of vascular injury.
The investigators enrolled patients diagnosed with HCC who were candidates for LMH and randomized them to undergo surgery with either the Glissonian or hilar dissection approach. Key metrics assessed included intraoperative blood loss, operation duration, postoperative complication rates, liver function recovery, and long-term oncological outcomes such as disease-free and overall survival. This robust study design aimed to resolve the clinical equipoise surrounding these methods.
Initial analyses revealed that the Glissonian approach conferred significant advantages in terms of reducing intraoperative blood loss. By controlling the portal triad en bloc, surgeons could achieve swift vascular occlusion, thereby minimizing hemorrhagic complications. The decreased need for extensive hilar manipulation also appeared to lower the incidence of inadvertent vascular injuries, a frequent concern in hilar dissection.
Conversely, the hilar dissection approach demonstrated strengths in offering enhanced visualization and differentiation of the individual portal elements. This precision is crucial for ensuring clear surgical margins and preserving uninvolved vascular and biliary structures. Notably, the dissection approach was associated with longer operative times, reflecting the meticulous nature of the technique, and slightly greater blood loss overall compared to the Glissonian method.
Postoperatively, patients in both groups exhibited comparable recovery trajectories regarding liver function normalization and complication rates, indicating that neither approach significantly compromised hepatic regeneration or patient safety. Importantly, the incidence of bile leaks and other common postoperative complications did not differ significantly between the two methods, underscoring their relative equivalence in immediate surgical outcomes.
Among the most compelling insights emerged from the long-term follow-up data, which included disease recurrence and survival rates. The study found no statistically significant differences in disease-free or overall survival between patients treated with Glissonian pedicle control versus those undergoing hilar dissection. This suggests that both techniques offer satisfactory oncological clearance when appropriately executed and highlight that surgical expertise may be a more decisive factor than the choice of approach.
Furthermore, the research team employed advanced laparoscopic imaging and intraoperative navigation tools, enhancing the procedural accuracy of both techniques. These technological adjuncts played a critical role in mitigating risks associated with hilar dissection and in confirming the adequacy of the Glissonian pedicle isolation, illustrating the evolving synergy between surgical innovation and clinical practice.
This study’s findings carry profound implications for surgical protocols in hepatobiliary oncology. By rigorously comparing two major LMH strategies, the research provides the surgical community with evidence-based guidance to tailor hepatic hilum management according to patient-specific anatomical and tumor-related factors. It also reinforces the notion that proficiency in both approaches is essential for optimizing outcomes in complex hepatic resections.
What sets this trial apart is its randomized, controlled design that reduces bias and variability inherent in retrospective surgical studies. The multi-center involvement and standardized operative procedures lend generalizability and robustness to the conclusions drawn. Moreover, the integration of detailed perioperative data with oncologic follow-up presents a comprehensive picture of the surgical impact.
The debate over the Glissonian versus hilar dissection approach has often hinged on theoretical advantage and individual surgeon preference. This pioneering trial grounds that discourse in measurable data, confirming that while the Glissonian approach expedites hepatic pedicle control and reduces blood loss, the hilar dissection method remains a valuable strategy for intricate anatomical situations demanding careful pedicle manipulation.
As minimally invasive hepatectomy continues to gain popularity worldwide due to enhanced recovery profiles and reduced hospital stays, studies like this underscore the importance of refining surgical techniques to maximize patient benefit. Surgeons are encouraged to consider their own experience, case complexity, and available technology when deciding on the hepatic hilum approach during LMH.
Future research may build upon these findings by exploring patient subgroups, such as those with cirrhosis or portal hypertension, to delineate which cohorts benefit most from each technique. Additionally, comparing these approaches in robotic-assisted hepatectomy contexts could unveil further nuances in surgical ergonomics and outcomes.
In summary, this groundbreaking randomized controlled trial decisively compares the extrahepatic Glissonian and hilar dissection approaches for hepatic hilum management in LMH for HCC patients. The evidence indicates that both approaches are viable, with the Glissonian approach offering operative efficiency and lower bleeding risk, while hilar dissection provides meticulous anatomical control. Crucially, long-term oncological outcomes appear unaffected by the choice of technique, spotlighting the paramount importance of surgical expertise and individualized patient care.
These discoveries mark a significant stride toward optimizing minimally invasive liver surgery and improving prognoses for patients battling hepatocellular carcinoma. As the field advances, embracing evidence-based surgical strategies will be key to delivering safer, more effective treatments that enhance quality of life and survival.
Subject of Research: Surgical approaches to hepatic hilum management during laparoscopic major hepatectomy in hepatocellular carcinoma patients.
Article Title: Laparoscopic extrahepatic Glissonian versus hilar dissection approach for major hepatectomy in patients with HCC: a randomized controlled trial.
Article References:
Peng, Y., Yang, Y., Chen, K. et al. Laparoscopic extrahepatic Glissonian versus hilar dissection approach for major hepatectomy in patients with HCC: a randomized controlled trial. Br J Cancer (2026). https://doi.org/10.1038/s41416-026-03458-2
Image Credits: AI Generated
DOI: 10.1038/s41416-026-03458-2
Tags: comparative efficacy of liver surgery methodsGlissonian approach in liver surgeryhepatocellular carcinoma surgical treatmenthilar dissection methodlaparoscopic major hepatectomy techniqueslong-term outcomes in hepatocellular carcinomaminimally invasive liver resectionportal triad control techniquesrandomized controlled trial in hepatectomyshort-term outcomes of liver surgerysurgical management of hepatic hilumvascular and biliary pedicle control