In an illuminating correction to a groundbreaking study published recently in BMC Cancer, researchers have revisited the outcomes of primary tumor resection in non-small cell lung cancer (NSCLC) patients presenting with pleural dissemination that was unexpectedly identified intraoperatively. This two-centre retrospective cohort study, led by Tao Bao and colleagues from various departments of thoracic and cardiothoracic surgery across prominent hospitals in Chongqing, China, delves into surgical decision-making nuances when pleural dissemination—a marker often signaling advanced metastatic spread—is found during surgery.
Non-small cell lung cancer continues to be the leading cause of cancer-related mortality globally, notorious for its heterogeneous presentation and unpredictable metastatic patterns. The discovery of pleural dissemination during thoracic surgery poses significant dilemmas. Traditionally, such cases are often deemed contraindications for curative surgery, favoring palliative treatments or systemic therapies instead. However, the cohort analyzed here challenges this convention by investigating the potential benefits of proceeding with primary tumor resection despite this unexpected finding.
The original study recruited patients treated at Daping Hospital and Xinqiao Hospital under the Army Medical University umbrella, alongside cases from the First Affiliated Hospital of Chongqing Medical University. The selection criteria highlighted NSCLC patients initially scheduled for curative resection but intraoperatively diagnosed with pleural dissemination—a scenario frequently excluded from randomized controlled trials due to its complexity.
Central to the study’s impact is the meticulous retrospective analysis of operative records, postoperative outcomes, and long-term survival data. The researchers engaged in detailed stratification considering tumor histology, stage, extent of pleural involvement, and adjuvant treatment modalities, thus painting a comprehensive picture of real-world clinical scenarios that surgeons and oncologists frequently encounter.
One of the pivotal revelations from this cohort is that carefully selected NSCLC patients with limited pleural dissemination who undergo primary tumor resection evidenced unexpectedly favorable survival outcomes compared to those who only received systemic therapies. This suggests that surgical intervention, even in the presence of pleural metastasis, could contribute to improved disease control and symptom management, potentially redefining surgical contraindications in such cases.
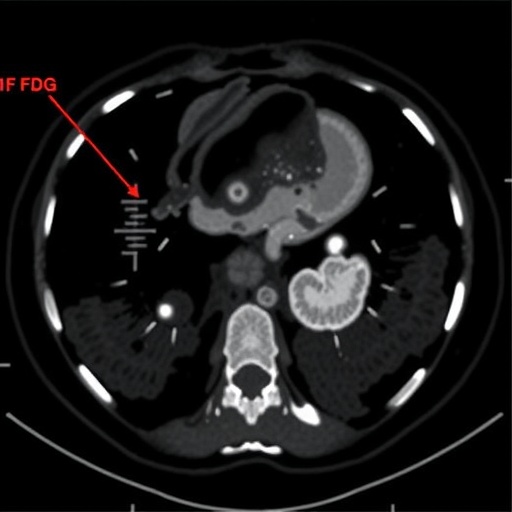
Moreover, intraoperative detection of pleural dissemination remains a diagnostic challenge, often reliant on a combination of visual assessment, frozen section biopsies, and pleural lavage cytology. The study emphasizes the importance of timely surgical judgment and highlights the role experienced thoracic surgeons play in determining operability and procedural extent when pleural involvement is ambiguous preoperatively.
Advancements in thoracoscopic techniques and perioperative imaging have augmented the capacity to identify and address pleural disease more precisely, yet this study underscores the ongoing necessity for an integrative approach. Multidisciplinary collaboration between thoracic surgeons, medical oncologists, radiologists, and pathologists remains paramount in tailoring patient-specific therapeutic pathways.
The retrospective nature of the research, while providing valuable insights, naturally invites caution in interpreting causality and generalizability. Nevertheless, it lays the groundwork for prospective trials and emphasizes the nuanced considerations in managing NSCLC patients encountering unexpected pleural dissemination during surgery.
The therapeutic implications extend into personalized medicine realms, where genomic profiling and molecular characterization of tumors could further stratify candidates for surgery versus systemic treatments. Targeted therapies and immunotherapies, increasingly becoming standard frontline options, complement surgical resection and could synergistically enhance survival and quality of life.
Crucially, the study impacts clinical guidelines by encouraging re-examination of rigid exclusion criteria for surgery in advanced NSCLC, advocating instead for a more individualized algorithm that weighs intraoperative findings against patient performance status, tumor biology, and anticipated response to adjunctive treatments.
The research team further elaborates on surgical techniques employed, noting that en bloc resection, combined with selective pleurectomy where feasible, can achieve macroscopic complete resection, essential for potential survival benefits. Their data also delineate postoperative morbidity and mortality rates, providing a realistic perspective on risks versus potential gains.
Importantly, the findings challenge entrenched dogma and encourage thoracic surgical teams globally to consider resection in select cases once pleural dissemination is unexpectedly discovered, potentially altering practice patterns and improving overall lung cancer management.
The correction issued to this study reaffirms the dedication to scientific rigor and transparency, ensuring that oncological and surgical communities have access to accurate data upon which to base critical clinical decisions. It highlights the iterative nature of research and the value of ongoing data validation.
In summary, this two-centre retrospective cohort study presents compelling evidence that primary tumor resection may offer survival and clinical benefits in NSCLC patients with intraoperatively detected pleural dissemination, advocating for a paradigm shift towards more aggressive surgical management in carefully selected cases, thereby opening new avenues in the war against lung cancer.
Subject of Research: Surgical outcomes of primary tumor resection in non-small cell lung cancer patients with pleural dissemination unexpectedly detected during operation
Article Title: Correction: Primary tumour resection in non-small cell lung cancer patients with pleural dissemination unexpectedly detected during operation: a two-centre retrospective cohort study
Article References: Bao, T., Deng, Y., Chen, L. et al. Correction: Primary tumour resection in non-small cell lung cancer patients with pleural dissemination unexpectedly detected during operation: a two-centre retrospective cohort study. BMC Cancer 25, 1398 (2025). https://doi.org/10.1186/s12885-025-14919-x
Image Credits: Scienmag.com
Tags: advancements in lung cancer researchcohort study on lung cancercurative surgery versus palliative careintraoperative findings in surgerymetastatic spread in lung cancernon-small cell lung cancer treatmentpleural dissemination in NSCLCprimary tumor resection outcomessurgical decision-making in cancerthoracic surgery interventionstumor removal in lung cancerunexpected benefits of surgery