Researchers from the University of Tsukuba show how tumors can disable the immune system to survive and grow
Credit: University of Tsukuba
Tsukuba, Japan – The goal of most cancers is to grow and take over the host’s body. The immune system has long been in the crosshairs of cancer researchers, as it plays a central role in defending the human body from foreign invasion. In a new study, researchers from the University of Tsukuba have revealed that tumors that produce a protein called soluble CD155 accumulate in the lungs of mice by disabling the immune system of the animals.
Soluble CD155 is a protein that is made by many different cells in the body and plays an important role in how cells migrate and develop. Surprisingly, several studies by the group at the University of Tsukuba have shown that higher serum levels of soluble CD155 can be found in patients with various types of cancer.
“Correlation does not imply causation,” says the corresponding author of the study and associate professor Kazuko Shibuya. “We wanted to know specifically how soluble CD155 is involved in the growth of cancer.”
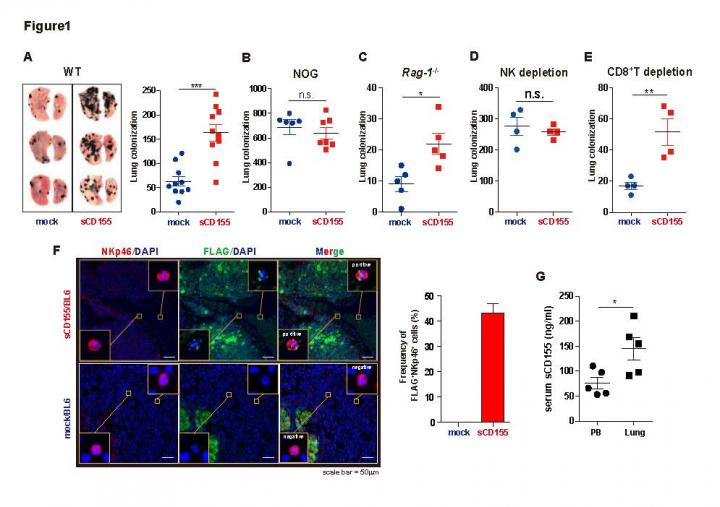
To function, proteins bind to other proteins. CD155 has been shown to bind to the proteins DNAM-1, TIGIT, and CD96, all of which are expressed by various types of immune cells. To achieve their goal, the researchers changed cancer cells, called B16/BL6 melanoma cells, to produce soluble CD155. When injected into normal mice or mice that are deficient in TIGIT or CD96, the soluble CD155-producing B16/BL6 cancer cells were able to settle and grow in their lungs, more so than compared with B16/BL6 cancer cells that had not been changed. Quite the opposite happened, however, when the same experiment was performed with mice deficient in DNAM-1–the researchers could not find a larger tumor in the lungs of the animals.
“Our results show that DNAM-1 was somehow involved in the tumor-promoting actions of soluble CD155,” says lead author of the study Genki Okumura. “Our next goal was to explore further how the two proteins interact to enable the growth of cancer”.
The researchers then depleted a certain type of immune cells, called natural killer (NK) cells, in the mice and found that all difference between the mice disappeared. In further experiments, they found that soluble CD155 prevented NK cells from releasing small proteins that are toxic to cancer cells by binding to DNAM-1.
“These are striking results that show how a single protein can drastically change the fate of a tumor. Targeting soluble CD155 could therefore be a new powerful strategy to treat cancer,” says Shibuya.
Given that tumor cells have to shield themselves from the immune system to grow, finding and disabling their ways to survive could mean defeating the growth and spread of cancer. Targeting soluble CD155 could mean an improved therapy for various types of cancer.
###
Media Contact
Naoko Yamashina
[email protected]
81-298-532-066
Related Journal Article
http://dx.




