Ryan Zurakowski, assistant professor of electrical and computer engineering at the University of Delaware, is co-author of a paper appearing in Nature Medicine on Jan. 12 highlighting the role of T-cells in HIV.
The paper, titled “HIV-1 Persistence in CD4+ T-Cells with Stem Cell-Like Properties,” provides evidence that a particular T-cell type may help researchers better understand why HIV can persist despite treatment.
Zurakowski’s co-authors include Mathias Lichterfeld, the paper’s lead author, and researchers from Massachusetts General Hospital (MGH); Ragon Institute of MGH, the Massachusetts Institute of Technology and Harvard University; the First Affiliated Hospital of China Medical University; Brigham and Women’s Hospital; and Howard Hughes Medical Institute.
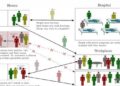
Zurakowski explained that HIV treatments do not kill infected cells. Instead, they stop the infection of new cells, and rely on the virus itself to kill the infected cells. Unfortunately, some cells infected by the virus — memory T-cells — are not killed by the virus.
T-cells are a type of lymphocyte, or white blood cell, produced by the thymus gland, that actively participates in the body’s immune response. “Memory” T-cells can live for years, or even decades, providing life-long immunity to previously encountered diseases. They can form “quiescent” infections, which last for years, and cause HIV to rebound whenever a patient stops treatment.
During a decade-long study, the researchers discovered that not all memory T-cells are alike. A subgroup of memory T-cells, called “Stem-Cell Memory T-cells” (Tscm), are different, particularly in their ability to produce daughter cells.
The researchers were able to show that the HIV-infected Tscm cells in patients on HIV therapy decayed more slowly than any other type of T-cell. As a result, after 10 years of therapy, the Tscm cells represented 24 percent of the total HIV infected cell population, despite being only 1 percent of the total T-cell population.
This finding is significant, Zurakowski said, because it demonstrates that Tscm cells are the slowest-decaying portion of the HIV reservoir.
“Over time this particular cell type plays an increasingly significant role in sustaining HIV infection in patients that have remained on therapy,” he said.
Zurakowski credits the finding to the diligence of Lichterfeld and the researchers at the Ragon Institute in carefully following the same HIV patients for a decade.
“Because the researchers have followed the same patients over a decade, we have created a high fidelity data set that would not otherwise have been possible,” he said.
Drugs currently being developed for cancer therapy that target stem-cell metabolic pathways may be able to target this cell type as well, due to the “stem-cell like” nature of the Tscm cells, he continued.
A better understanding of how the HIV virus leverages a cell’s stem cell-like properties of cellular immune memory to stay alive could lead to improved clinical strategies for HIV treatment.
“If we can find a way to selectively eliminate the HIV-infected Tscm cells, it will be a major step in developing a true ‘cure’ for HIV infection,” concluded Zurakowski.
Story Source:
The above story is based on materials provided by University of Delaware.