Drug class ‘notoriously difficult to quit,’ yet not intended for permanent use, according to authors in the journal of the american osteopathic association
Credit: JAOA
CHICAGO–February 20, 2020–Patients who have taken antidepressants for years should consider coming off the medication. However, researchers say they will likely face difficult and even dangerous withdrawal symptoms due to a physical dependence.
The best process is to follow a tapering schedule while consulting with a physician, according to research in The Journal of the American Osteopathic Association. Stopping medication outright is almost never advisable.
“I understand that many people feel safe in that their depression or anxiety is continuously managed by medication. However, these are mind-altering drugs and were never intended as a permanent solution,” says Mireille Rizkalla, PhD, Assistant Professor, Department of Clinical Integration at Midwestern University Chicago College of Osteopathic Medicine, and lead author on this research. “Once the patient’s depression or anxiety has been resolved, the physician should guide them toward discontinuation, while providing non pharmacologic treatments to help them maintain their mental health.”
Hard to quit
Patients who stop taking their medication often experience Antidepressant Discontinuation Syndrome (ADS), which includes flulike symptoms, insomnia, nausea, imbalance, sensory disturbances often described as electric shocks or “brain zaps”, and hyperarousal.
Older, first-generation antidepressants often come with additional risks for more severe symptoms, including aggressiveness, catatonia, cognitive impairment, and psychosis. Discontinuing any antidepressant also carries a risk for gradual worsening or relapsing of depression and anxiety, as well as suicidal thoughts.
Indefinitely medicated
A recent report from the CDC said a quarter of people taking antidepressants had been using them for a decade or more. Rizkalla says this data makes the case that patients and physicians are overly reliant on medication without concern for long-term consequences.
“I think we have a real problem with patient care management, when it comes to prescribing antidepressants,” says Rizkalla. “We tend to put patients on an SSRI and more or less forget about them.”
She adds that, while relatively safe, antidepressants still carry side effects, including weight gain, sexual dysfunction and emotional numbing. She also urges caution as the evidence for antidepressant risk factors is based on short-term usage, and says there are no sufficient longitudinal studies on the neurologic impact of taking antidepressants for decades.
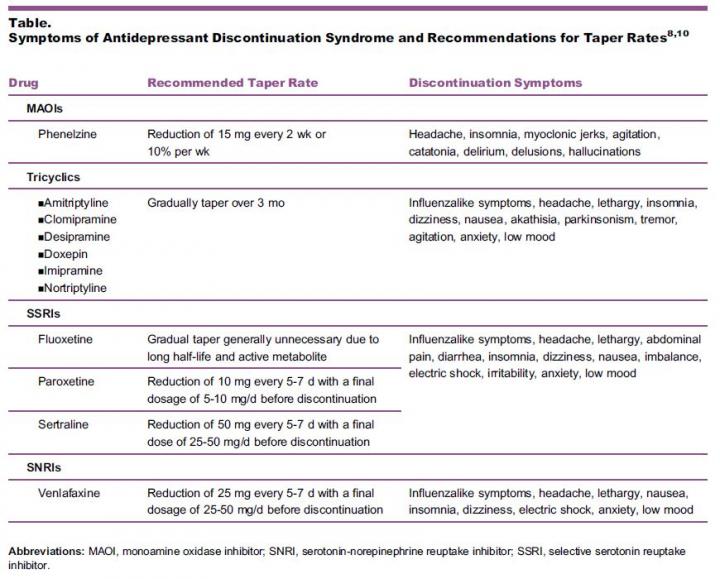
Rizkalla and her coauthors included the following tapering schedule for varying classes of antidepressants. However, she insists patients consult their physician before and throughout the process to monitor their symptoms and progress.
###
[See attached chart]
About The Journal of the American Osteopathic Association
The Journal of the American Osteopathic Association (JAOA) is the official scientific publication of the American Osteopathic Association. Edited by Robert Orenstein, DO, it is the premier scholarly peer-reviewed publication of the osteopathic medical profession. The JAOA’s mission is to advance medicine through the publication of peer-reviewed osteopathic research.
Media Contact
Jeff Brennan, Media Relations Manager
312-202-8161 | [email protected]
Media Contact
Jeff Brennan
[email protected]
312-202-8161
Related Journal Article
http://dx.




