Credit: Human Reproduction
Women who suffer from psychiatric disorders such as depression, anxiety, mania and schizophrenia following the live birth of their first child are less likely to go on to have more children, according to the first study to investigate this in a large nationwide population.
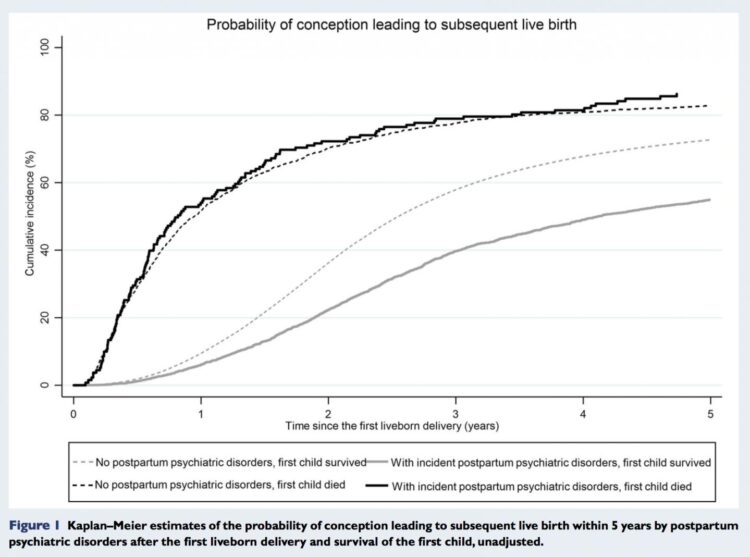
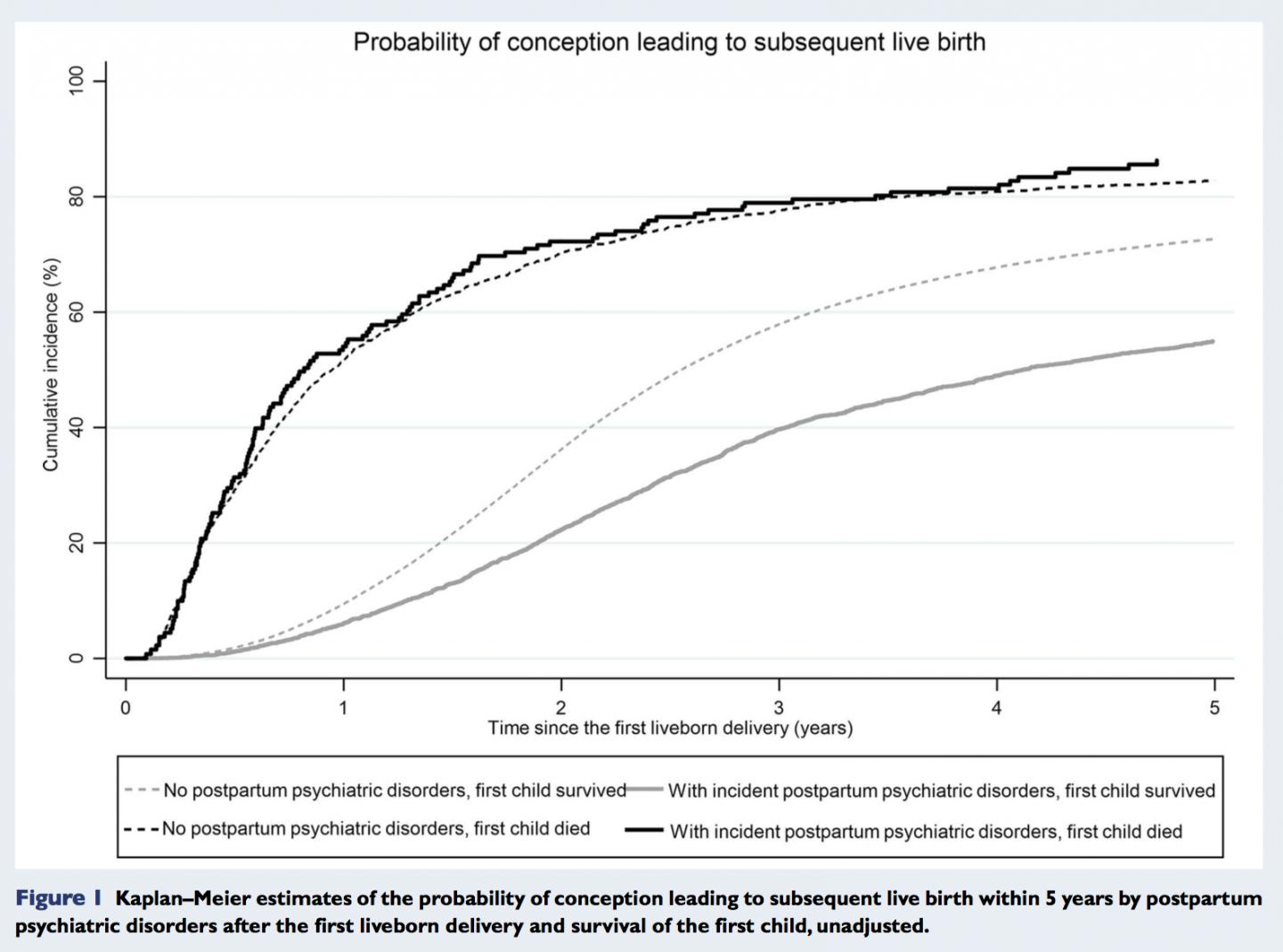
The study, which is published today (Monday) in Human Reproduction [1], one of the world’s leading reproductive medicine journals, found that 69% of women who experienced postpartum psychiatric disorders within the first six months after the birth of their first baby went on to have further children; this contrasts with 82% of mothers who did not experience psychiatric problems.
However, Dr Xiaoqin Liu, a post-doctoral researcher at the National Centre for Register-based Research at Aarhus University (Denmark), who led the study, said: “An important message to women who have a history of severe postpartum psychiatric disorders is that it is possible to prevent relapse. We recommend that they seek help from their family doctors or psychiatrists if they want to have another child, so that plans for treatment that are specific for their individual needs can be made to reduce the risk of relapse, and so that their health, well-being and symptoms can be closely monitored and treated.”
Previous research has shown that, overall, around three percent of women develop psychiatric disorders in the first three months after childbirth. These disorders encompass a wide range of mental health problems and usually involve a combination of abnormal thoughts, behaviours and relationships with other people. To date, there has been little research into whether or not this affects women’s subsequent reproduction.
Dr Liu said: “We wanted to explore whether women with postpartum psychiatric disorders had a reduced possibility of having a second child. Furthermore, we considered whether a reduction in the live birth rate was due to personal choices or decreased fertility, as these are important issues to consider.”
Dr Liu and her colleagues analysed data from Danish registries for 414,571 women who had their first live birth between 1997 and 2015 in Denmark. They followed the women for a maximum of 19.5 years until the next live birth, emigration, death, their 45th birthday or June 2016, whichever occurred first.
They identified women with postpartum psychiatric disorders by seeing if they were given prescriptions for psychotropic medications or had hospital contact for psychiatric disorders during the first six months after the live birth of their first child.
A total of 4,327 (1%) of women experienced psychiatric disorders following the birth of their first child. These women were a third less likely to have a second live birth compared to women who did not experience psychiatric disorders. If the first child died, the difference in subsequent live birth rates disappeared. However, if the psychiatric problem required hospitalisation, the likelihood of a woman having a second child nearly halved and this remained the case irrespective of whether the first child survived or not.
Dr Liu said: “Although fewer women with postpartum psychiatric disorders had subsequent children, it is noteworthy that about 69% of these women still chose to have a second child. For the remaining 31% of women, we need to differentiate the reasons why they did not have another child. If they avoided another pregnancy due to fear of relapse, an important clinical message to them is that prevention of relapse is possible.
“Women whose first child died were nearly four times as likely to have a subsequent live birth as women whose first child survived. These findings suggest that the overall reduced rate of subsequent live births among women who experienced psychiatric disorders after the birth of their first child is, at least in part, voluntary.”
The researchers say that other possible explanations for the reduction in the subsequent live birth rate may be that women with postpartum psychiatric disorders are less able to conceive or have more problematic relationships with partners.
“The reason why women with postpartum psychiatric disorders choose to have fewer children needs to be explored further,” said Dr Liu.
A limitation of the study is that, although the researchers had an almost complete follow-up of the women through the Danish registries, they did not have accurate information on stillbirths or miscarriages; only pregnancies that led to a live birth were included in the study. Another limitation is that not all women with psychiatric disorders might have received medications or hospital treatment. In addition, it might not be possible to generalise the findings of the study to populations in other countries.
“Denmark offers free and easily available healthcare to all individuals, so we believe our results can inform other, similar populations, although we cannot rule out local differences,” concluded Dr Liu.
###
[1] “Postpartum psychiatric disorders and subsequent live birth: a population-based cohort study in Denmark”, by Xiaoqin Liu et al. Human Reproduction journal. doi:10.1093/humrep/deaa016
Media Contact
Emma Mason
[email protected]
Related Journal Article
http://dx.