Between December 2024 and February 2025, a groundbreaking study was conducted at Semmelweis University in Budapest, where ten newborn infants suffering from moderate to severe hypoxic-ischemic brain injury received a novel treatment involving the intranasal administration of fresh breast milk. This pioneering therapeutic approach was designed to mitigate the long-term neurological consequences typically associated with neonatal brain damage caused by oxygen deprivation. The results of this clinical investigation, published recently in the prestigious journal Pediatric Research, part of the Nature portfolio, have opened new avenues for neonatal neuroprotection therapies, suggesting a safe and potentially transformative adjunct to the current standard care.
Hypoxic-ischemic encephalopathy (HIE) represents one of the most devastating clinical challenges in neonatal medicine, arising when the neonatal brain suffers from oxygen deprivation combined with restricted blood flow. This injury leads to both acute mortality and chronic neurological impairments, including cerebral palsy, cognitive disabilities, and epilepsy. Therapeutic hypothermia—lowering the infant’s body temperature to approximately 33–34°C—remains the only evidence-based treatment that can reduce mortality and improve neurological outcomes. However, the limitations and accessibility issues associated with cooling therapy underscore the need for innovative and complementary treatments.
The concept behind using breast milk as a neuroprotective agent stems from its rich composition of biologically active components, including stem cells, cytokines, growth factors, and neurotrophic substances. These elements have shown potential to support neurogenesis, reduce inflammation, and promote repair in damaged neural tissues. Unlike oral administration, the intranasal route capitalizes on the unique anatomical connection between the nasal mucosa and the central nervous system, allowing breast milk constituents to bypass the blood-brain barrier and directly access the brain through the olfactory and trigeminal nerve pathways.
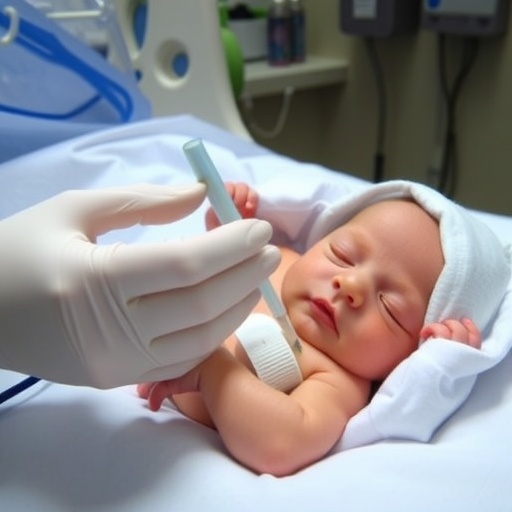
In the clinical protocol established at Semmelweis University, the treatment commenced within 48 hours after birth, coinciding with the critical therapeutic window for optimal neuroprotection in HIE. Fresh breast milk was meticulously collected from each infant’s mother and carefully administered into the nostrils under rigorous clinical supervision. The meticulous monitoring ensured the detection of any potential adverse respiratory or neurological reactions. Following the initial clinical phase, the therapy was transitioned to a home-based setting, wherein trained parents continued the intranasal administration for 28 consecutive days, supported by ongoing remote monitoring.
Remarkably, the study found no respiratory, circulatory, or neurological adverse events attributable to the intranasal breast milk treatment. This finding establishes a critical foundation for the safety profile of the procedure, affirming that breast milk, when delivered through the nasal passages, does not compromise neonatal physiological stability. This safety confirmation is a vital step before any large-scale efficacy trials can be pursued, providing reassurance to clinicians and families considering this innovative modality.
One of the notable obstacles encountered during the study was logistical rather than medical. The procurement and transport of breast milk from mothers residing in remote locations posed significant challenges. Dr. Ünőke Méder described instances where she personally traveled to distant, rural farms to collect milk, navigating difficult terrain where access was frequently impeded. These logistical complexities underscored not only the infrastructural demands of conducting such novel clinical research but also the psychosocial stress borne by families coping with traumatic early life events.
Supporting lactation among mothers who had undergone the emotional strain of a seriously ill newborn was another critical component of the study’s success. Initiating and maintaining breast milk expression under intense psychological pressure required specialized counseling and clinical support. This aspect highlighted the holistic nature of neonatal care, where maternal well-being and infant treatment strategies are deeply interconnected and must be addressed simultaneously to optimize outcomes.
From the parental perspective, engagement was more positive than initially anticipated. As Dr. Eszter Tarjányi noted, many parents found empowerment and solace in contributing directly to their infant’s care during a period fraught with uncertainty. Learning the precise technique for intranasal administration proved straightforward once the parents understood that the process was painless and safe for their child. This unexpected ease of parental involvement could play a crucial role in the future scalability and acceptability of the therapy.
The current research focuses exclusively on establishing the safety of intranasal breast milk administration in clinically and home-monitored environments. While the biological rationale and preclinical animal models are compelling, the effectiveness and long-term neurological benefits of this therapy remain to be rigorously evaluated in larger, controlled clinical trials. Existing studies from Germany and Canada on preterm infants with brain hemorrhages have previously hinted at potential neuroprotective effects of intranasal breast milk, lending preliminary clinical credence to this approach.
Should subsequent investigations confirm efficacy, intranasal breast milk therapy could revolutionize neonatal care, particularly in resource-limited settings where conventional cooling therapy is unavailable or impractical. The simplicity, cost-effectiveness, and biological compatibility of using a mother’s own fresh milk as a therapeutic agent would offer a sustainable, low-risk approach to addressing neonatal brain injury worldwide. Moreover, this method could extend neuroprotective care beyond hospital walls, integrating into home healthcare frameworks.
International interest in this therapeutic concept is already growing, with several countries exploring opportunities to adapt and implement the intranasal breast milk protocol. Such global collaborations would facilitate the collection of broader clinical data, drive standardized training programs for families and healthcare providers, and address cultural and infrastructural barriers. Through these efforts, intranasal breast milk therapy may emerge as a critical component of comprehensive neonatal neuroprotection strategies.
In summary, the research conducted at Semmelweis University pioneers a promising frontier in neonatal therapeutic interventions. By harnessing breast milk’s unique biological potential and combining it with innovative delivery methods, clinicians are charting a path toward safer, more accessible, and efficacious treatments for newborns afflicted by hypoxic-ischemic brain injuries. Establishing safety in real-world settings lays the groundwork for future studies that could ultimately transform global health outcomes for this vulnerable population.
Subject of Research: Neonatal hypoxic-ischemic brain injury and intranasal breast milk therapy
Article Title: Intranasal Breast Milk as a Novel Neuroprotective Treatment for Brain-Injured Newborns: A Safety Study
News Publication Date: Early 2025
Web References:
Study published in Pediatric Research: https://www.nature.com/articles/s41390-026-04847-2
DOI: 10.1038/s41390-026-04847-2
Image Credits: Semmelweis University, Budapest, Hungary
Keywords: Hypoxic-ischemic encephalopathy, neonatology, intranasal therapy, breast milk, neuroprotection, therapeutic hypothermia, brain injury, neonatal care, stem cells, neurotrophic factors, clinical safety, home-based therapy
Tags: adjunct therapies for neonatal carebreast milk neuroprotective propertieshypoxic-ischemic encephalopathy therapyinnovative neonatal medicine Hungaryintranasal breast milk therapyneonatal brain injury treatmentneonatal hypoxic-ischemic brain damageneuroprotection for newbornsnovel treatments for HIEpediatric neurorehabilitationSemmelweis University clinical studytherapeutic hypothermia alternatives