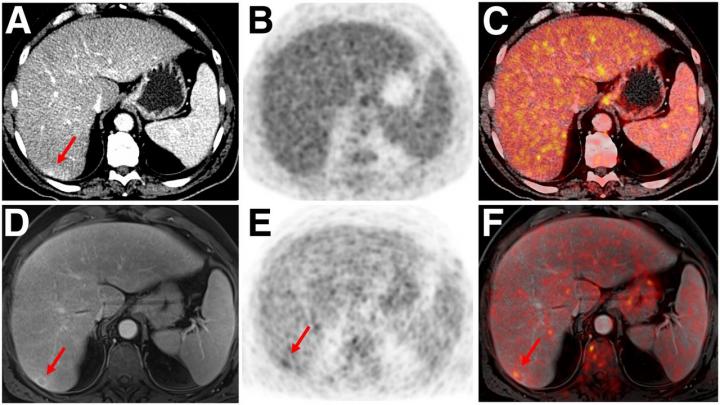
Credit: Images created by Ole Martin, University Dusseldorf, Medical Faculty and Benedikt Schaarschmidt, University Hospital Essen.
Reston, VA–A single-center observational study of more than 1,000 oncological examinations has demonstrated that positron emission tomography/magnetic resonance imaging (PET/MRI) facilitates cancer staging as well as PET/computed tomography (PET/CT) and improves lesion detectability in select cancers, potentially helping to promote fast, efficient local and whole-body staging in one step. The study, published in The Journal of Nuclear Medicine, also shows that PET/MRI significantly reduces overall radiation exposure when compared to PET/CT–of particular benefit to pediatric and adolescent patients.
While PET/CT is known as the diagnostic cornerstone in various oncologic imaging guidelines due to its sensitivity and high-resolution morphologic imaging, PET/MRI has higher soft-tissue contrast and lower radiation exposure. However, clinical data for PET/MRI are scarce due to the lack of clinical studies with relevant sample sizes.
In the observational study, a total of 1,003 whole-body PET/MRI examinations on 918 patients from a single center were compared with whole-body PET/CT examinations of the same patients. The oncological indications included lung cancer, gastrointestinal cancer or neuroendocrine cancer, gynecologic or breast cancer, prostate cancer, lymphoma, melanoma, head and neck cancer, cancer of unknown primary and malignant bone disease.
Board-certified nuclear medicine physicians and radiologists evaluated the examinations to identify additional findings on PET/MRI that were missing on PET/CT and probable diagnoses; additional but indeterminate findings on PET/MRI requiring additional examinations or follow-up; classification of indeterminate findings on PET/CT by PET/MRI; and missed findings on PET/MRI in comparison to PET/CT. Effective dose of both modalities was also investigated.
Additional information on PET/MRI was reported for 26.3 percent of examinations, compared with PET/CT. Of these, additional malignant findings were detected in 5.3 percent, leading to a change in TNM staging in 2.9 percent due to PET/MRI. Definite lesion classification of indeterminate PET/CT findings was possible in 11.1 percent with PET/MRI. In 2.9 percent, lesions detected on PET/CT were not visible on PET/MRI. Malignant lesions were missed in 1.2 percent on PET/MRI, leading to a change in TNM staging in 0.5 percent. The estimated mean effective dose for whole-body PET/CT amounted to 17.6 ± 8.7 mSv, in comparison to 3.6 ± 1.4 mSv for PET/MRI, resulting in a potential dose reduction of 79.6 percent.
“Due to the higher soft tissue contrast, PET/MRI improves lesion detection and reduces the need for additional examinations in comparison to PET/CT,” said Benedikt Schaarschmidt, MD, professor and radiologist at the University Hospital Essen in Essen, Germany. “Especially in younger patients who need repeated diagnostic procedures, our data advocate the use of PET/MRI due to the markedly reduced radiation exposure of PET/MRI when compared to PET/CT.”
He continued, “Hybrid imaging examinations are now part of complex diagnostic algorithms in multiple cancer types. Based on our data, PET/MRI could be an important adjunct to PET/CT by providing diagnostic advantages and improving diagnostic algorithms in numerous cancers at the same time. Furthermore, the markedly reduced radiation exposure of PET/MRI could lead to a more frequent use of this examination in oncological patients, most notably for treatment monitoring.”
###
The authors of “PET/MRI Versus PET/CT for Whole-Body Staging: Results from a Single-Center Observational Study on 1,003 Sequential Examinations” include Ole Martin, Julian Kirchner, Philipp Heusch and Gerald Antoch, Department of Diagnostic and Interventional Radiology, University of Dusseldorf, Medical Faculty, Dusseldorf, Germany; Benedikt M. Schaarschmidt, Saravanabavaan Suntharalingam, Johannes Grueneisen, Aydin Demircioglu, Michael Forsting and Lale Umutlu, Department of Diagnostic and Interventional Radiology and Neuroradiology, University Hospital Essen, University of Duisburg-Essen, Essen, Germany; Harold H. Quick, Erwin L. Hahn Institute for Magnetic Resonance Imaging, University of Duisburg-Essen, Essen, Germany, and High-Field and Hybrid MR Imaging, University Hospital Essen, University of Duisburg-Essen, Essen, Germany; and Ken Herrmann, Department of Nuclear Medicine, University Hospital Essen, University of Duisburg-Essen, Essen, Germany.
This study was made available online in December 2019 ahead of final publication in print in August 2020.
Please visit the SNMMI Media Center for more information about molecular imaging and precision imaging. To schedule an interview with the researchers, please contact Rebecca Maxey at (703) 652-6772 or [email protected].
About the Society of Nuclear Medicine and Molecular Imaging
The Journal of Nuclear Medicine (JNM) is the world’s leading nuclear medicine, molecular imaging and theranostics journal, accessed close to 10 million times each year by practitioners around the globe, providing them with the information they need to advance this rapidly expanding field. Current and past issues of The Journal of Nuclear Medicine can be found online at http://jnm.
JNM is published by the Society of Nuclear Medicine and Molecular Imaging (SNMMI), an international scientific and medical organization dedicated to advancing nuclear medicine and molecular imaging–precision medicine that allows diagnosis and treatment to be tailored to individual patients in order to achieve the best possible outcomes. For more information, visit http://www.
Media Contact
Rebecca Maxey
[email protected]
Original Source
http://www.
Related Journal Article
http://dx.




