Stem cells from the dental pulp of wisdom teeth can be coaxed to turn into cells of the eye’s cornea and could one day be used to repair corneal scarring due to infection or injury, according to researchers at the University of Pittsburgh School of Medicine. The findings, published online today in STEM CELLS Translational Medicine, indicate they also could become a new source of corneal transplant tissue made from the patient’s own cells.
James Funderburgh, Ph.D., professor of ophthalmology at Pitt and associate director of the Louis J. Fox Center for Vision Restoration of UPMC and the University of Pittsburgh
Corneal blindness, which affects millions of people worldwide, is typically treated with transplants of donor corneas, said senior investigator James Funderburgh, Ph.D., professor of ophthalmology at Pitt and associate director of the Louis J. Fox Center for Vision Restoration of UPMC and the University of Pittsburgh, a joint program of UPMC Eye Center and the McGowan Institute for Regenerative Medicine.
“Shortages of donor corneas and rejection of donor tissue do occur, which can result in permanent vision loss,” Dr. Funderburgh said. “Our work is promising because using the patient’s own cells for treatment could help us avoid these problems.”
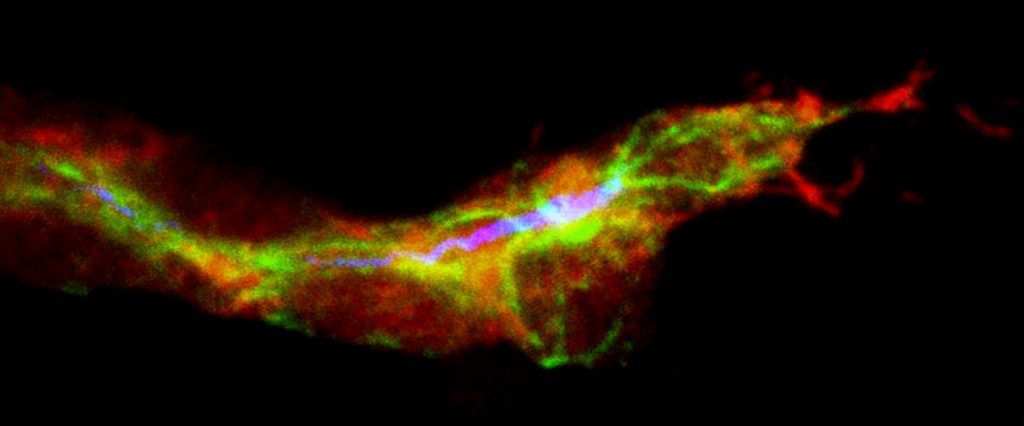
Experiments conducted by lead author Fatima Syed-Picard, Ph.D., also of Pitt’s Department of Ophthalmology, and the team showed that stem cells of the dental pulp, obtained from routine human third molar, or wisdom tooth, extractions performed at Pitt’s School of Dental Medicine, could be turned into corneal stromal cells called keratocytes, which have the same embryonic origin.
The team injected the engineered keratocytes into the corneas of healthy mice, where they integrated without signs of rejection. They also used the cells to develop constructs of corneal stroma akin to natural tissue.
“Other research has shown that dental pulp stem cells can be used to make neural, bone and other cells,” Dr. Syed-Picard noted. “They have great potential for use in regenerative therapies.”
In future work, the researchers will assess whether the technique can correct corneal scarring in an animal model.
Story Source:
The above story is based on materials provided by University of Pittsburgh School of Medicine.