Glioblastoma multiforme (GBM) represents one of the most lethal and aggressive forms of brain cancer predominantly diagnosed in adults, challenging the limits of current therapeutic modalities. Affecting approximately 30,000 individuals annually in the United States, GBM carries a dismal prognosis, with a five-year survival rate lingering around a mere 7 percent. Current clinical management strategies—surgical resection, radiation therapy, and chemotherapeutic intervention using temozolomide—while standard, fail to offer curative potential. The invasive and heterogeneous nature of GBM tumors, coupled with difficulties in drug delivery across the protective blood-brain barrier, underscores the urgent need for innovative treatment approaches.
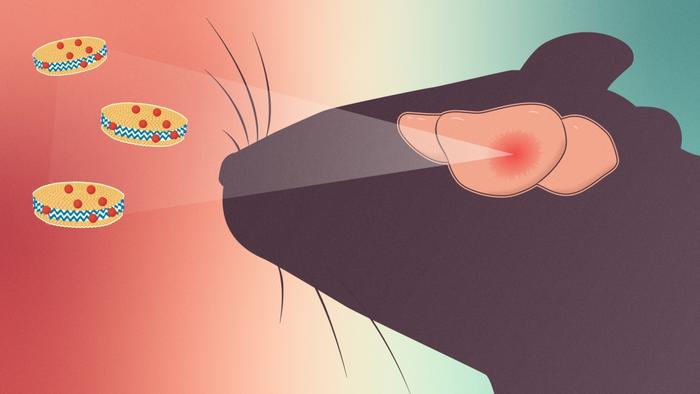
Recent groundbreaking research out of the University of Michigan sheds new light on a promising therapeutic avenue that harnesses the power of nanotechnology. Scientists have engineered specialized nanodiscs capable of targeting cholesterol metabolism within GBM tumors—effectively starving malignant cells and enhancing survival outcomes in murine models. This novel approach pivots on the metabolic vulnerabilities of GBM cells, which rely heavily on external cholesterol uptake due to their inability to synthesize adequate levels de novo. By interrupting this crucial supply line, the nanodiscs impair tumor growth and promote cancer cell death.
To circumvent the limitations of systemic chemotherapy, which often induces considerable toxicity and off-target effects, the research team concentrated on local delivery of the nanodiscs. By injecting these particles into the tumor cavity immediately following surgical tumor debulking, the approach maximizes drug concentration at the site of residual disease. This locoregional administration not only diminishes systemic side effects but also ensures that nanodiscs act directly within the brain’s microenvironment where they are needed most, overcoming the blood-brain barrier challenge.
Moreover, the study demonstrated a synergistic effect when nanodisc treatment was combined with conventional radiation therapy. Radiation remains a central pillar in GBM management, yet it is insufficient on its own due to the tumor’s resilient nature. When administered adjunctively, the nanodiscs boosted therapeutic efficacy, increasing survival beyond what radiation alone could achieve. Notably, more than 60 percent of treated mice survived long term after this combined regimen, a significant improvement compared to controls.
In parallel, the nanodiscs were functionalized with immunostimulatory CpG oligonucleotides on their surface, designed to awaken and amplify the body’s immune response to tumor antigens. This dual therapeutic mechanism not only targets cancer metabolism but also mobilizes adaptive immunity, fostering the recruitment and activation of immune cells that can recognize and destroy tumor cells. The immunological memory established by this treatment confers protection against tumor rechallenge, as evidenced by about 68 percent of mice successfully rejecting a subsequent tumor implantation.
This interplay between metabolic inhibition and immune activation represents a cutting-edge paradigm in cancer therapy. By leveraging the multifaceted roles of nanodiscs—both as delivery vehicles and immunomodulators—the treatment addresses the complex biology of GBM tumors more comprehensively than traditional modalities that focus on singular targets or pathways. It’s a strategy designed to outpace tumor adaptability and heterogeneity, minimizing the chances of recurrence which remains the primary driver of mortality in GBM patients.
The implications for clinical translation are profound. The University of Michigan team has initiated scale-up processes for nanodisc synthesis and is laying the groundwork for upcoming clinical trials. Such a transition will require rigorous validation of safety, pharmacokinetics, and efficacy in humans, yet the preclinical findings offer a beacon of hope for transforming GBM treatment landscapes in the near future. Achieving meaningful improvements in patient survival while preserving neurological function remains the ultimate goal.
Equally noteworthy is the interdisciplinary collaboration that fueled this research—from cancer biologists decoding tumor metabolism to pharmaceutical scientists specializing in nanoparticle engineering. This convergence of expertise underscores the necessity of cross-domain partnerships to tackle complex diseases like GBM, where simplistic approaches have failed. The integration of nanomedicine, immunology, and neurosurgery paves the way for innovative therapeutic designs that can be personalized and adapted to individual patient needs.
In summary, the development of HDL-mimetic nanodiscs loaded with Liver X Receptor agonists signifies a major leap forward in the fight against glioblastoma multiforme. By cutting off cholesterol supply critical for tumor growth and simultaneously activating the immune system, this dual-action therapy extends survival and reduces recurrence in animal models. If these findings translate effectively to human patients, they could herald a paradigm shift in brain cancer treatment, offering renewed hope for a disease historically marked by therapeutic failure.
Subject of Research: Animals
Article Title: HDL Nanodiscs Loaded with Liver X Receptor Agonist Decreases Tumor Burden and Mediates Long-term Survival in Mouse Glioma Model
News Publication Date: 18-Apr-2025
Web References:
DOI: 10.1002/smll.202307097
References:
“HDL Nanodiscs Loaded with Liver X Receptor Agonist Decreases Tumor Burden and Mediates Long-term Survival in Mouse Glioma Model,” Small
Image Credits: University of Michigan
Keywords:
Health and medicine; Glioblastomas; Brain tumors; Nanoparticles
Tags: blood-brain barrier and drug deliverychallenges in treating brain tumorscholesterol metabolism in cancer cellsenhancing survival rates in GBMinnovative therapies for glioblastoma multiformeLXR agonists for cancer therapymetabolic vulnerabilities of glioblastomamurine models in cancer studiesnanoparticles in glioblastoma treatmentnanotechnology in cancer researchtargeted drug delivery for brain cancerUniversity of Michigan cancer research