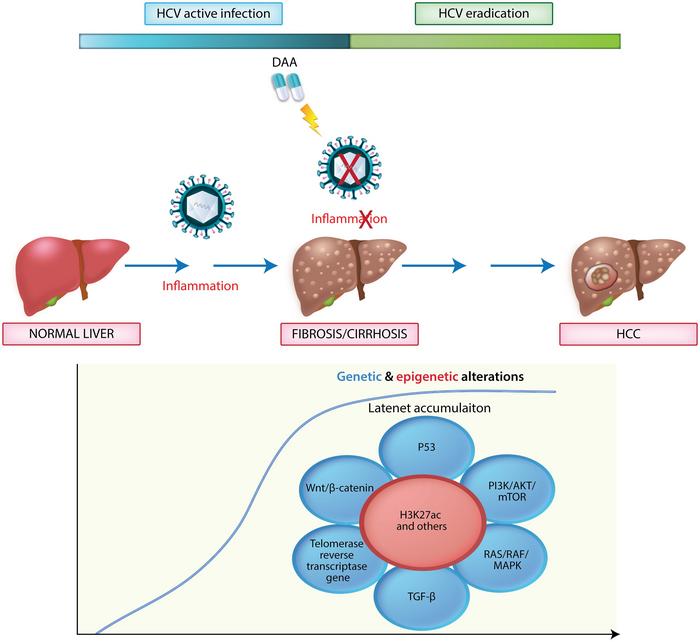
The advent of direct-acting antivirals (DAAs) has marked a significant turning point in the management of hepatitis C virus (HCV) infections, presenting a groundbreaking advancement that not only enhances treatment efficacy but also alters the long-term outcomes for patients. As millions grapple with the repercussions of chronic HCV, understanding the implications of these treatments on the incidence of hepatocellular carcinoma (HCC) becomes imperative. The dynamics between viral eradication through DAAs and the subsequent risk of HCC are complex, as recent findings reveal that while DAAs succeed in eliminating the virus, the shadow of HCC risk looms for certain cohorts, particularly those with pre-treatment cirrhosis or advanced fibrosis.
It’s crucial to acknowledge at the outset that achieving sustained virologic response (SVR) is a game-changer in HCV treatment. SVR, defined as the absence of detectable HCV RNA in a patient’s blood for a certain period post-treatment, correlates directly with reduced mortality and morbidity associated with HCV. However, what complicates this narrative is the lingering threat of HCC, particularly in patients who present with cirrhosis or significant fibrosis prior to initiating DAA therapy. As these patients achieve SVR, studies indicate that they remain susceptible to HCC, necessitating a re-evaluation of current surveillance strategies to ensure optimal patient outcomes.
Historically, surveillance strategies for HCC have been well-established for patients with cirrhosis. However, the question of how to approach surveillance in patients with F3 or bridging fibrosis (advanced fibrosis) post-SVR is still open for debate. Various guidelines from international liver associations propose differing recommendations, adding to the complexity of clinical decision-making in this area. For instance, while the European Association for the Study of the Liver (EASL) advocates for semi-annual surveillance for patients with F3 fibrosis, the American Association for the Study of Liver Diseases (AASLD) is less definitive, suggesting that the cost-effectiveness of such monitoring remains uncertain unless additional risk factors are present.
A pivotal aspect of this discourse is the underlying mechanisms that contribute to HCC development even after viral eradication in HCV patients. It has become increasingly evident that chronic HCV infection induces genetic and epigenetic changes that may persist post-SVR. For instance, studies have identified alterations in oncogenic pathways involving the telomerase reverse transcriptase (TERT) gene, Wnt/β-catenin signaling, and the p53 pathway as crucial players in hepatocarcinogenesis. The implications of these findings necessitate further scrutiny of patient cohorts who, despite achieving SVR, may harbor genetic predispositions increasing their likelihood of developing HCC.
Moreover, the relationship between metabolic health and HCC risk in post-SVR patients cannot be overstated. Patients with comorbid conditions such as diabetes mellitus, obesity, and dyslipidemia have shown heightened HCC risk, exacerbating concerns for those previously infected with HCV. Alcohol consumption further compounds this risk, acting synergistically with underlying metabolic disorders to increase the incidence of HCC in susceptible individuals. This interplay underscores the need for a tailored approach to risk stratification in HCV-cured patients, wherein individual factors are assessed comprehensively to determine the necessity and frequency of ongoing surveillance.
The discordance in surveillance recommendations highlights a critical need for healthcare providers to stay well-informed of evolving evidence and adopt a flexible, individualized approach to patient care. Factors such as the patient’s age, the presence of fibrosis, and elevated post-treatment alpha-fetoprotein (AFP) levels will serve as pivotal guiding parameters in establishing risk profiles. These individualized assessments are critical for determining the optimal frequency of imaging and blood tests aimed at early HCC detection.
Additionally, emerging research exploring the transcriptomic landscape of patients who achieve SVR reveals retained signatures associated with HCC risk. The persistence of these molecular markers post-treatment suggests that while viral eradication is an important milestone, it is not a definitive end point. Instead, ongoing surveillance that incorporates advanced biomarker evaluations may be necessary to mitigate the risk of HCC development in higher-risk patients.
Clinically, the goal remains to balance the benefits of proactive surveillance against the burden of unnecessary interventions in lower-risk groups. In doing so, healthcare professionals must draw from an eclectic mix of clinical evidence to guide their recommendations, including outcomes from recent cohort studies and meta-analyses that elucidate the long-term effects of DAA therapies. With patient-centered care at the forefront, ongoing dialogues within the medical community will remain essential as we navigate the complexities presented by HCV eradication and its ramifications for hepatocellular carcinoma.
In conclusion, the transformative capabilities of DAAs in revolutionizing HCV treatment usher forth a new era of possibilities; however, the specter of HCC underscores an urgent need for sustained vigilance and research. Investigations into genetic risk factors, combined with the meticulous evaluation of post-treatment health, will be paramount in crafting effective surveillance models for HCV-cured patients. As we move forward, ensuring that individualized care pathways are prioritized in clinical practice will lead to improved outcomes and a future where the burden of HCC is significantly reduced.
Subject of Research: Hepatocellular carcinoma risk post-HCV eradication with Direct-acting Antivirals
Article Title: Beyond the Cure: Navigating Hepatocellular Risk and Surveillance after Hepatitis C Eradication in the Direct-acting Antiviral Era
News Publication Date: 8-Feb-2025
Web References: Journal of Clinical and Translational Hepatology
References: DOI: 10.14218/JCTH.2024.00499
Image Credits: Credit: Ashwani K. Singal, Chencheng Xie
Keywords: Hepatocellular carcinoma, Hepatitis C, Direct-acting antivirals, Liver, Cirrhosis, Surveillance, Genetic predisposition, Personalized medicine, Oncogenic pathways.
Tags: antiviral therapy and liver cancerchronic hepatitis C patient carecirrhosis and fibrosis considerationsdirect-acting antivirals impactHCC risk in treated patientshepatitis C treatment outcomeshepatocellular carcinoma risk managementimplications of viral eradication on HCClong-term HCV management strategiesmonitoring liver health after DAApost-eradication surveillance strategiessustained virologic response significance