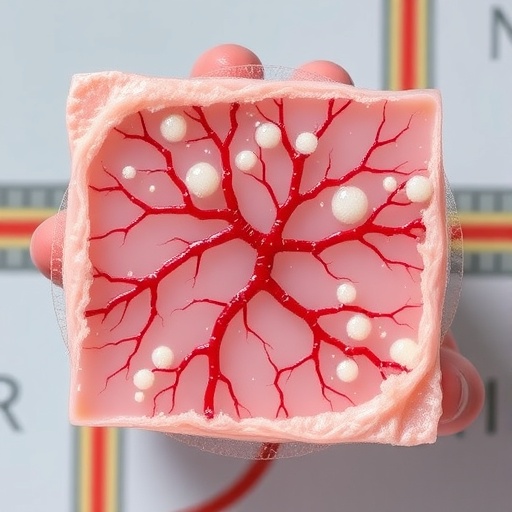
In a groundbreaking advancement set to transform the landscape of liver transplantation and regenerative medicine, scientists at the Terasaki Institute for Biomedical Innovation have engineered a vascularized liver tissueoid-on-a-chip (LToC) platform that authentically replicates the intricate human liver environment. Spearheaded by Dr. Vadim Jucaud and his team, this innovative platform perfectly recapitulates critical structural, functional, and immunological characteristics of human liver tissue, providing an unprecedented avenue for studying liver regeneration and immune-mediated allograft rejection within a human-relevant and dynamically vascularized system.
Liver transplantation continues to stand as the definitive clinical solution for patients suffering from end-stage liver disease. However, advancing our understanding of transplant biology, particularly the immune mechanisms underlying graft rejection and the pathways central to tissue repair and regeneration, has been severely constrained by the absence of physiologically precise human model systems. Traditional cell cultures and animal models fall short in replicating the liver’s complex multicellular architecture, its sophisticated vasculature network, and the dynamic immunological milieu that governs transplant fate, presenting a formidable barrier to translational progress.
Addressing these formidable challenges, the research team developed a liver tissueoid from donor-matched human hepatic progenitor cells in conjunction with intrahepatic portal vein endothelial cells. Cultured within a dynamic perfusion bioreactor, this co-culture self-organized into a perfusable microvascular network within merely one week. This initial vasculogenesis was succeeded by a progressive maturation stage extending over 49 days, culminating in a functional liver-mimetic tissueoid exhibiting salient features akin to native liver tissue.
Throughout long-term culture, the vascularized liver tissueoid demonstrated sustained viability and preserved endothelial integrity, as validated by advanced imaging and immunofluorescence methods. Functionally, the tissueoid exhibited hallmark hepatic activities — notably synthesizing albumin and urea at physiologically relevant levels, secreting key complement factors, and producing hepatocyte growth factor (HGF), a critical mediator of liver regeneration. These activities collectively confirmed the platform’s capacity to emulate native hepatic function over extended periods in vitro.
Beyond functional validation, comprehensive cellular phenotyping revealed that the mature tissueoid harbored a broad repertoire of liver-relevant cell populations. These included parenchymal hepatocytes, ductal cholangiocytes, resident macrophage-like Kupffer cells, fibrogenic stellate cells, and a robust endothelial network, replicating the cellular heterogeneity and spatial organization inherent to human liver tissue. This intricate multicellularity underpins the platform’s suitability for studying complex cell–cell and cell–immune system interactions central to transplant biology.
Crucially, the LToC system was employed to simulate immune-mediated allograft rejection by introducing allogeneic T cells into the perfused tissueoid. This immune challenge reproduced key features of acute cellular rejection: notable decline in overall tissue viability, disruption of the endothelial lining, and loss of hepatic lineage markers. Immunologically, there was an upregulation of HLA class I molecules and a surge in pro-inflammatory cytokines such as IL-6, TNF-α, IL-1β, and IFN-γ. Additionally, elevated levels of cytotoxic effector molecules—granzyme A, granzyme B, and perforin—were observed, mirroring the immunopathologic signature seen in clinical transplant rejection.
This integrative platform’s ability to model the interplay between hepatic tissue regeneration and immune activation marks a significant stride toward understanding the mechanistic basis for transplant outcomes in a human-specific context. According to Dr. Abdul Rahim Chethikkattuveli Salih, the first author on the study, “The liver tissueoid-on-a-chip enables us to recreate critical aspects of liver tissue regeneration and immune-mediated rejection with a level of complexity and physiological relevance not previously achievable.”
Dr. Vadim Jucaud, Principal Investigator and Assistant Professor, emphasized the system’s translational potential, remarking, “By integrating a rich vascular network, diverse liver cell populations, and robust immune responsiveness in a single microscale platform, our liver tissueoid-on-a-chip supports a deeper mechanistic study of transplant immunobiology. This approach opens exciting possibilities for preclinical evaluation of immunosuppressive therapies and the development of highly personalized treatment regimens for liver transplant patients.”
The innovation advances the legacy of Dr. Paul I. Terasaki, renowned for his monumental contributions to transplantation immunology. As one of Dr. Terasaki’s last doctoral mentees, Dr. Jucaud underscores the personal and professional significance of this work: “Dr. Terasaki’s vision that translational innovation must ultimately improve patient well-being guides our efforts. Our work bridges bioengineering, immunology, and regenerative medicine, moving toward practical solutions with tangible clinical impact.”
The liver tissueoid-on-a-chip platform reflects a broader paradigm shift in biomedical research that embraces sophisticated organotypic models to overcome the limitations of animal studies and simplistic cultures. By faithfully reproducing human tissue complexity and immune dynamics, this technology accelerates drug discovery, enhances mechanistic insights, and drastically reduces the translational gap between bench and bedside.
The Terasaki Institute continues its commitment to patient-centric innovation, advancing integrative technologies like the LToC platform that promise to revolutionize transplant medicine and liver disease treatment. By fostering interdisciplinary collaboration across engineering, immunology, and clinical science, the Institute aims to usher in a new era of personalized and precision medicine tailored to the unique immunological landscape and regenerative capacity of individual patients.
As the scientific community seeks to tackle the complexities of organ transplantation, the vascularized liver tissueoid-on-a-chip stands out as a pivotal tool for dissecting fundamental biological processes, evaluating novel therapeutics, and ultimately improving long-term transplant success rates and patient quality of life. This breakthrough epitomizes how cutting-edge tissue engineering intersects with immunology to reshape the future of regenerative medicine and transplantation biology.
Subject of Research: Human tissue samples
Article Title: Liver Tissueoid on-a-Chip Modeling Liver Regeneration and Allograft Rejection
News Publication Date: February 18, 2026
Web References: DOI: 10.1002/adma.202521178
Image Credits: Terasaki Institute for Biomedical Innovation
Keywords
Transplantation, Organ transplantation, Liver regeneration, Immunology, Biomedical engineering, Personalized medicine
Tags: dynamic perfusion bioreactorhepatic progenitor cell culturehuman liver microenvironmentimmune-mediated allograft rejectionintrahepatic portal vein endothelial cellsliver regeneration researchliver tissue engineeringliver transplant biologyliver transplant rejection modelregenerative medicine liver modelsvascularized liver tissueoid-on-a-chipvascularized tissue models