WHAT:
A drug approved to treat certain autoimmune diseases and cancers successfully alleviated symptoms of a rare genetic syndrome called autoimmune polyendocrine syndrome type 1 (APS-1). Researchers identified the treatment based on their discovery that the syndrome is linked to elevated levels of interferon-gamma (IFN-gamma), a protein involved in immune system responses, providing new insights into the role of IFN-gamma in autoimmunity. The study, led by researchers at the National Institutes of Health’s National Institute of Allergy and Infectious Diseases, was published today in the New England Journal of Medicine.
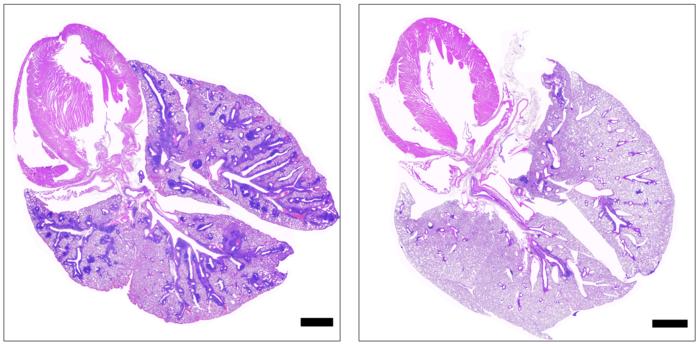
Credit: NIAID
WHAT:
A drug approved to treat certain autoimmune diseases and cancers successfully alleviated symptoms of a rare genetic syndrome called autoimmune polyendocrine syndrome type 1 (APS-1). Researchers identified the treatment based on their discovery that the syndrome is linked to elevated levels of interferon-gamma (IFN-gamma), a protein involved in immune system responses, providing new insights into the role of IFN-gamma in autoimmunity. The study, led by researchers at the National Institutes of Health’s National Institute of Allergy and Infectious Diseases, was published today in the New England Journal of Medicine.
In a three-stage study, conducted in mice and people, the researchers examined how APS-1 causes autoimmune disease. The syndrome is marked by dysfunction of multiple organs, usually beginning in childhood, and is fatal in more than 30% of cases. This inherited syndrome is caused by a deficiency in a gene that keeps the immune system’s T cells from attacking cells of the body, leading to autoimmunity; chronic yeast infections in the skin, nails, and mucous membranes; and insufficient production of hormones from endocrine organs, such as the adrenal glands. Symptoms include stomach irritation, liver inflammation, lung irritation, hair loss, loss of skin coloring, tissue damage, and organ failure.
In the first stage of this study, researchers led by scientists in NIAID’s Laboratory of Clinical Immunology and Microbiology examined the natural history of APS-1 in 110 adults and children. Blood and tissues were analyzed to compare gene and protein expression in people with and without APS-1. They found elevated IFN-gamma responses in the blood and tissues of people with APS-1, indicating that IFN-gamma may play an important role in the disease and providing a pathway to target for treatment.
In the second stage of the study, the scientists examined mice with the same gene deficiency that causes APS-1 in people, finding that the animals also experienced autoimmune tissue damage and elevated IFN-gamma levels. Mice also deficient in the gene for IFN-gamma did not have autoimmune tissue damage, which showed a direct link between IFN-gamma and APS-1 symptoms. With this understanding, the researchers looked for a drug that could be used to lower IFN-gamma activity in people. They selected ruxolitinib, a Janus kinase inhibitor, because it acts by shutting down the pathway driven by IFN-gamma. When ruxolitinib was administered to the mice with the gene deficiency that causes APS-1, IFN-gamma responses were normalized and T cells were prevented from infiltrating tissues and damaging organs. These results showed that ruxolitinib could alleviate effects of the gene deficiency, suggesting that it could be effective for treatment of APS-1 in people.
The researchers administered ruxolitinib, which was supplied by the NIH Clinical Center, to five people—two adults and three children—with APS-1 in the third stage of the study. The dosing and regimens were tailored to the individuals, and the treatments were continued for over a year. The drug was safe and tolerated well, and improvement in symptoms was seen in all study participants. Blood and tissue analyses revealed decreased production of IFN-gamma from T cells, as well as normalized levels of IFN-gamma in the blood. Many APS-1-related symptoms were reduced, including hair loss, oral yeast infections, stomach and bowel irritation, hives, and thyroid inflammation.
The results revealed that normalizing IFN-gamma levels using ruxolitinib could reduce the damaging effects of APS-1 in people. The scientists note that a study with a larger and more diverse group of patients is needed to determine whether ruxolitinib and similar drugs are suitable treatments for individuals with APS-1. They write that understanding the role of IFN-gamma in autoimmunity may lead to the development of treatments for related diseases. This research highlights the importance of finding the causes of and treatments for rare diseases.
Editorial note: APS-1 is also known as polyendocrinopathy-candidiasis-ectodermal dystrophy (APECED) in the literature.
REFERENCE:
V Oikonomou et al. The role of interferon-gamma in Autoimmune Polyendocrine Syndrome Type 1. New England Journal of Medicine DOI: 10.1056/NEJMoa2312665 (2024).
WHO:
Michail S. Lionakis, M.D., Sc.D., chief of NIAID’s Fungal Pathogenesis Section and deputy chief of NIAID’s Laboratory of Clinical Immunology and Microbiology, is available to discuss this research.
CONTACT:
To schedule interviews, please contact NIAID News & Science Writing Branch, 301-402-1663, [email protected].
NIAID conducts and supports research—at NIH, throughout the United States, and worldwide—to study the causes of infectious and immune-mediated diseases, and to develop better means of preventing, diagnosing and treating these illnesses. News releases, fact sheets and other NIAID-related materials are available on the NIAID website.
About the National Institutes of Health (NIH): NIH, the nation’s medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit http://www.nih.gov/.
NIH…Turning Discovery Into Health®
Journal
New England Journal of Medicine
DOI
10.1056/NEJMoa2312665




