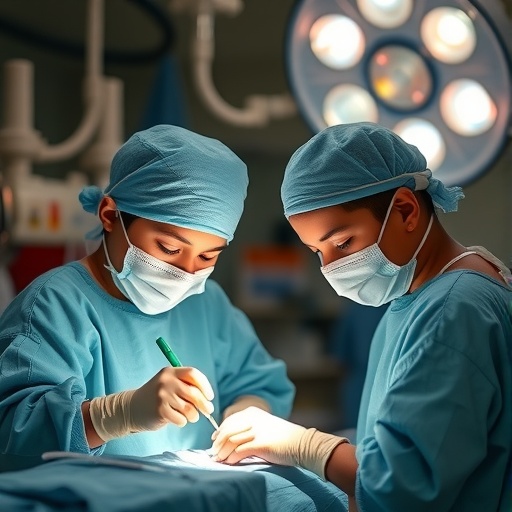
Children requiring immediate, life-saving abdominal surgery following traumatic injuries face dramatically different survival prospects depending on the economic status of the country in which they receive treatment. An extensive global study led by researchers at the University of Cambridge has uncovered a stark disparity, revealing that children in lower-income countries are nearly six times more likely to die within thirty days after emergency trauma laparotomy than their counterparts in more affluent nations. This groundbreaking research highlights critical global health inequalities in pediatric trauma care and calls for urgent transformation of trauma systems to address these unmet pediatric needs.
The investigation, published in The Lancet Child & Adolescent Health, analyzed data from 237 children aged 18 and under who underwent emergency laparotomy due to severe abdominal trauma. This cohort spanned 85 hospitals distributed across 32 countries, making it one of the largest international datasets examining surgical outcomes in pediatric trauma to date. The metabolic and physiological responses of children to trauma markedly differ from adults, necessitating specialized approaches in both emergency medicine and surgery. Yet, many trauma systems worldwide are primarily designed around adult care models.
Traumatic injury remains one of the leading causes of death and subsequent disability among children and adolescents globally. The mechanisms of injury frequently include road traffic collisions, interpersonal violence, and accidental harm. The study focused explicitly on children suffering from severe abdominal injuries, whose care pathways—from injury scene to surgical intervention—were meticulously compared across diverse healthcare environments. The results demonstrate a stark contrast in the speed, quality, and resources allocated for pediatric trauma care in lower versus higher-income settings.
The overall mortality rate observed in the study was 8%, but this figure masks extreme variations between countries at different stages of economic development. After controlling for confounding factors such as injury severity and patient characteristics, researchers found a nearly sixfold increase in mortality risk for children treated in less developed countries. This discrepancy is alarming and suggests systemic shortcomings in trauma care infrastructure, resource distribution, and clinical capabilities within these nations.
One central issue identified by the study was the prolonged delay children experienced before hospital arrival and definitive surgical treatment in lower-income countries. Timeliness is a critical determinant in trauma outcomes, particularly in abdominal injuries where hemorrhage control and vital organ preservation are paramount. Moreover, children in these environments were significantly less likely to receive essential interventions such as blood transfusions, computed tomography (CT) scans for accurate injury assessment, and administration of tranexamic acid to mitigate bleeding. The diminished involvement of consultant surgeons further compromised surgical care quality.
Additionally, the proportion of pediatric trauma cases was notably higher in poorer countries, which indicates a multifold challenge. These regions face a dual burden: a larger pediatric population suffering traumatic injuries requiring emergency surgery and fewer resources to address this growing healthcare demand. This double jeopardy underscores the urgent need for targeted investment in child-specific trauma care services and broader public health initiatives to prevent injuries.
Professor Timothy Hardcastle of the University of KwaZulu-Natal, a co-author of the study, emphasizes the complexity of these challenges, which span the entire trauma care continuum. From the moment a child suffers an injury through the transport to hospital, surgical intervention, intensive care admission, and eventual recovery, numerous systemic gaps contribute to preventable mortality. Access to blood transfusion services and advanced critical care, often limited in resource-constrained settings, are critical bottlenecks affecting survival rates.
Perhaps most pivotal is the recognition that trauma care systems historically have neglected the unique medical needs of children. Pediatric patients are not simply miniature adults; anatomical, physiological, and developmental differences necessitate specialized equipment, personnel trained in pediatric trauma management, and tailored clinical protocols. Dr. Michael Bath, co-lead author and University of Cambridge expert, stresses that many global trauma infrastructures have yet to be recalibrated to accommodate these essential distinctions.
Trauma treatment for children demands rapid access to pediatric emergency resuscitation, diagnostic imaging appropriately scaled to their size, and surgical teams proficient in child-focused laparotomy techniques. Post-operative intensive care must also be attuned to pediatric-specific requirements, including fluid management, nutritional support, and rehabilitation services, which are frequently inadequate in under-resourced hospitals. The absence of these elements contributes significantly to elevated morbidity and mortality.
The study advocates for a comprehensive overhaul of trauma care frameworks worldwide, urging governments, health ministries, and international agencies to allocate resources specifically for pediatric trauma services. Enhancement strategies should encompass ensuring age-appropriate medical devices, implementing referral pathways optimized for children, and extensive workforce training to improve clinical competencies in pediatric emergency and surgical care. Bolstering access to critical interventions such as blood products, CT imaging, and senior clinical oversight could be transformative.
Significant investments in healthcare infrastructure and education are paramount to closing the survival gap illuminated by the research. Improving pediatric trauma outcomes mandates a systemic approach incorporating injury prevention, emergency response optimization, surgical capacity building, and rehabilitation. The convergence of dedicated clinical protocols and resource availability tailored to the pediatric population has the potential to save thousands of young lives each year globally.
This landmark study serves as a clarion call to reconceptualize trauma management through the lens of child-centered care. As pediatric trauma continues to impose a heavy burden on global child health, especially in low- and middle-income countries, the research underscores the ethical imperative to design trauma systems that reflect the physiological and developmental nuances of children, ensuring equitable access to life-saving interventions around the world.
Tags: child abdominal trauma treatmentchildren emergency surgery survival rateseconomic impact on child surgery survivalemergency laparotomy in childrenglobal pediatric surgical outcomeshealthcare inequalities in pediatric traumainternational pediatric surgery studylife-saving surgery in low-resource settingslow-income countries health outcomespediatric trauma care disparitiespediatric trauma systems improvementtrauma surgery mortality rates