In a groundbreaking study set to redefine our understanding of a prevalent form of stroke, scientists have uncovered compelling evidence that challenges the traditional notion linking fatty artery deposits to lacunar ischemic stroke. This insight not only reshapes the pathology associated with this condition but also sheds light on why conventional antiplatelet therapies, such as aspirin, often underperform in preventing these specific strokes.
Lacunar ischemic stroke, which accounts for approximately 25% of all ischemic strokes in the United Kingdom annually, has long been attributed to the accumulation of atherosclerotic plaques in large arteries. However, the latest research conducted by teams from the University of Edinburgh alongside the UK Dementia Research Institute and international collaborators reveals a divergent vascular pathology underlying this stroke subtype. The study pivots focus from fatty arterial blockages to the microvascular architecture within the brain itself, particularly emphasizing arterial enlargement and elongation.
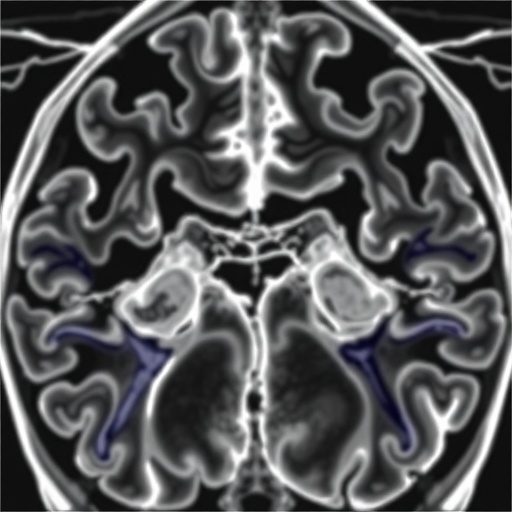
This novel vascular abnormality—marked by the dilatation and tortuosity of cerebral small arteries—correlates strongly with the incidence of lacunar stroke, suggesting a distinct mechanistic pathway from that of other ischemic strokes. Detailed magnetic resonance imaging (MRI) analyses performed immediately post-stroke and during a one-year follow-up period enabled researchers to monitor cerebrovascular changes, the evolution of small vessel disease, and the development of new cerebral lesions.
Their data decisively demonstrated that while large artery stenosis was predominantly linked to non-lacunar strokes, it bore minimal association with lacunar pathology or the progression of small vessel damage. Conversely, patients exhibiting pronounced arterial widening within the brain were found to have over a fourfold increased likelihood of presenting lacunar stroke. This arterial remodeling was further implicated in an exacerbated burden of small vessel disease and accelerated brain tissue injury.
One of the study’s most striking revelations was the frequent emergence of silent cerebral infarcts—microscopic brain injuries caused by covert disruptions in blood supply that escape clinical detection. Despite adherence to standard stroke preventive therapies, more than 25% of study participants developed these subtle yet cumulatively detrimental lesions within the follow-up timeframe. This phenomenon underscores the inadequacy of current treatments focused mainly on platelet aggregation inhibition in halting microvascular degeneration.
The implications for clinical management are profound; the classical model centered on combating atherothrombotic large vessel occlusion must be supplemented or supplanted by strategies targeting the intrinsic abnormalities of cerebral small vessels. This paradigm shift has already catalyzed interventional trials such as the LACunar Intervention Trial 3 (LACI-3), which explores the efficacy of pharmacologic agents like cilostazol and isosorbide mononitrate. These drugs, long utilized in cardiovascular contexts, are being repurposed to reinforce microvascular resilience, potentially attenuating subsequent stroke risk and mitigating cognitive deterioration.
Professor Joanna Wardlaw, a leading expert in neuroimaging and cerebrovascular disease at the University of Edinburgh, highlighted the critical distinction established by this research. She emphasized that the failure of antiplatelet drugs in lacunar stroke prevention is attributable to their misdirected therapeutic target; rather than large artery plaque, the primary pathology resides within the small vessel milieu. This recognition propels a renewed sense of urgency to innovate treatments that directly address the microangiopathic processes responsible.
The study—published in the eminent journal Circulation—draws on an observational cohort of 229 stroke patients subjected to rigorous clinical and cognitive scrutiny, supplementing traditional assessments with cutting-edge neuroimaging techniques. The comprehensive analysis affords a nuanced understanding of cerebrovascular remodeling and its clinical sequelae, delineating a clear path forward for research and therapeutic development.
Moreover, the international collaborative effort, involving researchers from China and Mexico, reflects the global significance of lacunar stroke as a contributor to long-term disability, dementia, and recurrent cerebrovascular events. Understanding and mitigating small vessel disease could profoundly alter patient trajectories worldwide, reducing the burden on healthcare systems and improving quality of life for millions.
This study’s findings catalyze a reassessment of stroke pathology and prevention, urging neurologists, researchers, and pharmaceutical developers to pivot toward cerebral microvascular health. As LACI-3 and similar trials progress, there is cautious optimism that targeted therapeutics may finally stem the tide against lacunar stroke and its devastating consequences.
Ultimately, this research revamps the clinical landscape of ischemic stroke, prioritizing microvascular pathology and challenging entrenched paradigms. The emphasis on arterial widening rather than narrowing as a critical biomarker heralds a transformative leap forward in stroke science, opening avenues for precision medicine and new hope for affected individuals.
Subject of Research: People
Article Title: [Not provided within the text]
News Publication Date: 6-May-2026
Web References: http://dx.doi.org/10.1161/CIRCULATIONAHA.126.079493
References: Circulation Journal: 10.1161/CIRCULATIONAHA.126.079493
Image Credits: [Not provided within the text]
Keywords: Health and medicine
Tags: artery dilation in strokecerebral small artery tortuositylacunar ischemic stroke risklimitations of antiplatelet therapy in strokemicrovascular pathology in strokeMRI analysis of cerebrovascular changesnon-atherosclerotic stroke mechanismsnovel insights into ischemic strokestroke risk factors beyond atherosclerosisUK Dementia Research Institute stroke studyUniversity of Edinburgh stroke researchvascular abnormalities in brain stroke