In a recent correspondence published in Nature Communications, researchers M. Albayram and O. Albayram present a compelling response to prior observations concerning hyperintense FLAIR signals localized within the anterior cranial fossa. This discussion is rooted deeply in the nuances of neuroimaging techniques, with a focus on the interpretation and diagnostic implications of FLAIR (Fluid-Attenuated Inversion Recovery) MRI sequences, which have become indispensable in the evaluation of various intracranial pathologies.
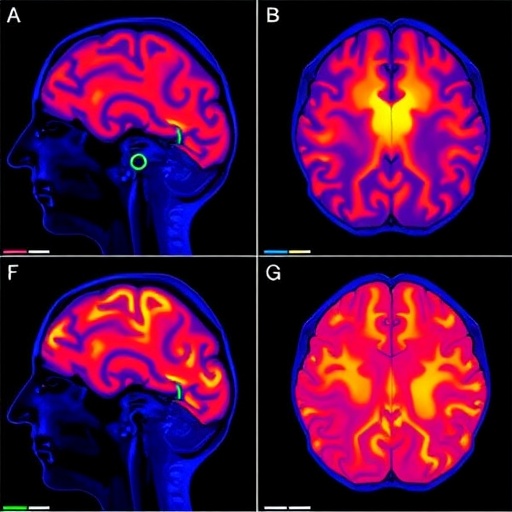
FLAIR MRI has revolutionized neurodiagnostic imaging by allowing for the suppression of cerebrospinal fluid (CSF) signals, thereby enhancing the visibility of lesions, edema, and other pathological changes adjacent to CSF spaces. The anterior cranial fossa—a critical region housing essential frontal lobe structures—has recently been under scrutiny due to reported hyperintense signals in FLAIR sequences, findings that have raised questions about their pathological or physiological origin.
The correspondence meticulously addresses these hyperintense signals, emphasizing the need to differentiate between true pathological changes and benign variants or imaging artifacts. The authors underscore that such high-intensity signals within the anterior cranial fossa may not necessarily indicate disease processes and that an accurate interpretation requires integrating clinical findings, detailed imaging protocols, and a thorough understanding of regional anatomy.
Technically, the hyperintense FLAIR signal can emerge due to variations in tissue composition, CSF flow dynamics, or even technical parameters of MRI acquisition, such as inversion times and echo times. The Albayrams highlight the importance of optimizing MRI protocols to minimize artifacts and improve differentiation between pathological and non-pathological hyperintensities. They suggest advanced imaging techniques, including high-resolution scans and potential use of complementary sequences, to further elucidate these ambiguous signals.
From a pathological perspective, hyperintense FLAIR signals in the anterior cranial fossa have been associated with processes such as meningitis, encephalitis, subarachnoid hemorrhage, and neoplastic infiltration. However, the reply warns against overinterpretation without corroborative clinical or imaging evidence, as normal anatomic variations—such as arachnoid granulations or vascular structures—can mimic disease.
The correspondence also ventures into the realm of CSF physiology, detailing how alterations in CSF flow or subtle inflammatory changes can manifest as hyperintense signals. The authors propose that certain patterns of signal increase may reflect transient, non-pathological states influenced by factors like hydration status, patient positioning, or even recent intracranial pressure fluctuations.
In addressing potential diagnostic pitfalls, the authors advocate for a multimodal imaging approach. They recommend correlating FLAIR findings with diffusion-weighted imaging (DWI), contrast-enhanced sequences, and, where applicable, MR angiography or venography to distinguish vascular contributions from inflammatory or neoplastic processes. They further elucidate how discrepancies between these modalities can guide clinical decision-making and patient management strategies.
Furthermore, the authors illuminate the role of artificial intelligence and machine learning in the prospective analysis of MRI data. By training algorithms on large datasets incorporating normal variants and pathological states, future neuroimaging may achieve higher specificity in characterizing ambiguous hyperintense signals, minimizing diagnostic uncertainty.
The reply also touches upon the importance of longitudinal imaging follow-up. Serial MRI studies can provide invaluable insight into the evolution or resolution of hyperintense FLAIR signals, distinguishing transient benign phenomena from progressive disease. This approach reinforces the notion that imaging findings must be contextualized within a temporal framework and clinical scenario.
Integral to this nuanced interpretation is an enhanced understanding of the histopathological correlates of hyperintense FLAIR signals. The correspondence encourages ongoing histological investigations to define how cellular and extracellular matrix alterations translate into MRI signal variances at a microstructural level.
The discussion extends to potential therapeutic implications. Misinterpretation of hyperintense FLAIR signals could lead to unnecessary interventions ranging from invasive biopsies to inappropriate pharmacologic treatments. Accurate delineation, therefore, is critical for optimizing patient outcomes and avoiding iatrogenic complications.
In addition to clinical considerations, the authors reflect on the broader implications for neuroimaging standards and guidelines. They call for refined imaging protocols tailored to the anterior cranial fossa and emphasized education for radiologists and clinicians about recognizing the spectrum of normal and abnormal FLAIR appearances.
The reply concludes by advocating for collaborative research integrating neuroradiology, neuropathology, and computational imaging. They envision a future where precision imaging and multidisciplinary approaches foster rapid and accurate diagnoses, improving prognostication and personalized patient care.
This insightful correspondence by M. and O. Albayram thus offers a pivotal reassessment of hyperintense FLAIR signals in the anterior cranial fossa. Their analysis enhances our understanding of this enigmatic finding, encouraging a balanced interpretation that integrates technical imaging properties, physiological factors, and clinical context—an endeavor that continually advances the precision of neuroimaging diagnostics.
Subject of Research: Interpretation of hyperintense FLAIR MRI signals in the anterior cranial fossa and their clinical and technical implications.
Article Title: Reply to: Hyperintense FLAIR signal in the anterior cranial fossa.
Article References:
Albayram, M., Albayram, O. Reply to: Hyperintense FLAIR signal in the anterior cranial fossa. Nat Commun 17, 4060 (2026). https://doi.org/10.1038/s41467-026-72195-0
Image Credits: AI Generated
DOI: https://doi.org/10.1038/s41467-026-72195-0
Tags: anterior cranial fossa imaging findingscerebrospinal fluid suppression techniquesclinical implications of FLAIR MRIdifferentiating pathological vs benign FLAIR signalsFLAIR MRI sequence diagnostic usefrontal lobe neuroimaging abnormalitieshyperintense FLAIR signals in brain MRIinterpretation of intracranial hyperintensitiesMRI imaging protocols for brain lesionsneurodiagnostic imaging advancementsneuroimaging artifacts in FLAIR sequencesregional brain anatomy in MRI analysis