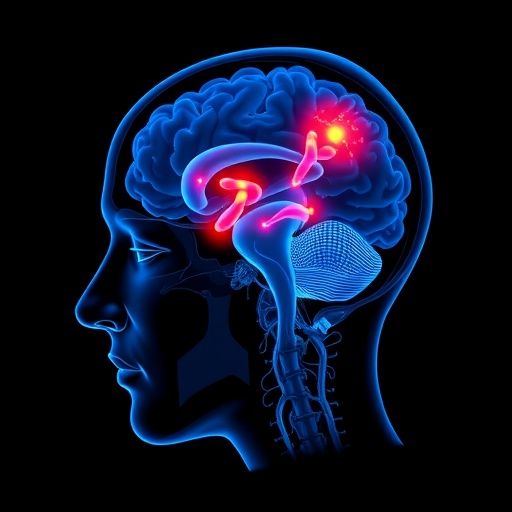
For over two decades, the scientific consensus attributed the most severe form of narcolepsy primarily to the degeneration of hypocretin-producing neurons located in the hypothalamus. This understanding shaped much of the diagnostic framework and therapeutic approaches surrounding the disorder. However, a groundbreaking study by researchers at UCLA Health, recently published in Nature Communications, challenges this long-held view by revealing that the pathophysiology of narcolepsy with cataplexy is far more complex than previously believed, involving not one but two distinct neuronal populations.
In their extensive investigation, the UCLA team utilized postmortem brain tissue from individuals diagnosed with narcolepsy accompanied by cataplexy, as well as neurologically healthy controls. The study uncovered compelling evidence of significant neuronal loss not only in the hypothalamus but also within the locus coeruleus, a pivotal brainstem nucleus responsible for synthesizing norepinephrine. This bi-regional degeneration suggests that narcolepsy’s hallmark symptoms—excessive daytime sleepiness and sudden episodes of muscle weakness—may be linked to a concurrent breakdown of two critical neural circuits rather than a singular neurochemical deficiency.
Historically, narcolepsy type 1, characterized by debilitating daytime somnolence and cataplexy, has been explained chiefly through the lens of hypocretin deficiency. Hypocretin, also known as orexin, is a neuropeptide instrumental in promoting wakefulness and arousal, synthesized by neurons situated in the lateral hypothalamus. The targeted loss of these neurons was believed to be the central pathological event causing the disorder. Yet, this new research suggests that the involvement of the locus coeruleus—which sends projections both upward to cortical regions and downward to spinal motor neurons to regulate muscle tone and arousal—provides a more comprehensive explanation for the complex clinical manifestations of narcolepsy.
Quantitative analyses revealed that in narcoleptic individuals, norepinephrine-producing neurons within the locus coeruleus were reduced by an average of 46% compared to controls, with some showing losses as high as 66%. Intriguingly, surviving neurons appeared hypertrophic, enlarging by approximately 18%. This hypertrophy might represent a compensatory mechanism by which the remaining cells strive to maintain noradrenergic signaling despite marked cell loss. Such morphological plasticity underscores the dynamic nature of the locus coeruleus network in the narcoleptic brain.
In addition to neuronal degeneration, the study documented pronounced neuroinflammatory changes within the locus coeruleus. Microglial cells, the brain’s resident immune sentinels, were observed to be more than twice as abundant and significantly enlarged in patients. This robust microglial activation mirrors similar inflammatory responses previously noted surrounding hypocretin neurons in the hypothalamus, bolstering the hypothesis of an immune-mediated component in narcolepsy’s pathogenesis. The findings align with the known genetic associations implicating immune system involvement, particularly genes linked to antigen presentation and autoimmunity.
Crucially, the nature of the neuronal loss appears to be distinct from classical neurodegenerative disorders such as Parkinson’s or Alzheimer’s diseases. The locus coeruleus neurons in narcolepsy patients demonstrated minimal accumulation of hallmark pathological protein aggregates such as alpha-synuclein and tau, indicating that the mechanisms driving cell death diverge from those identified in these more extensively studied neurodegenerative diseases. Although small deposits of these proteins were detected, their sparse presence compels further research to elucidate their potential role, if any, in narcolepsy’s etiology.
To determine whether the locus coeruleus degeneration was a secondary consequence of hypocretin cell loss, the researchers examined animal models, including genetically engineered mice and narcoleptic dogs. These models exhibited a profound loss of hypocretin neurons consistent with narcolepsy phenotypes but displayed no significant reduction in locus coeruleus neurons. This disparity emphasizes that, at least in humans, damage to the brainstem norepinephrine system is not an epiphenomenon of hypothalamic degeneration but rather a parallel pathological hallmark, highlighting the complexity of narcolepsy’s neural underpinnings.
Adding a new dimension to longstanding diagnostic conundrums, the dual-system hypothesis may explain why a subset of narcolepsy patients—estimated at 15-30%—exhibit normal cerebrospinal fluid hypocretin levels despite clinically manifesting cataplexy. The involvement of an additional degenerative locus coeruleus pathway raises the possibility that these cases represent a distinct biological subtype, challenging existing classification frameworks and necessitating revised diagnostic criteria incorporating locus coeruleus integrity assessments.
The therapeutic implications of this revelation are profound. Current pharmacological treatments for narcolepsy often aim to enhance wakefulness by targeting hypocretin-related pathways. However, drugs that elevate norepinephrine activity, such as reboxetine and solriamfetol, have shown notable efficacy in ameliorating symptoms. This clinical observation coheres with the study’s elucidation of locus coeruleus degeneration, suggesting that bolstering noradrenergic signaling could mitigate both excessive sleepiness and muscle atonia episodes. Such insights pave the way for the development of more targeted and perhaps combinatorial therapeutic strategies addressing multiple neural substrates.
Dr. Jerome Siegel, senior author of the study and director of UCLA’s Center for Sleep Research, emphasizes that these findings do not negate the established role of hypocretin deficiency but rather expand the neuropathological landscape of narcolepsy. “We have, until now, been examining only part of the picture,” he states. Comprehensive understanding of the full scope of neuronal alterations promises to unlock novel avenues for diagnosis and intervention, ultimately improving patient outcomes.
Methodologically, the team’s meticulous approach involved analyzing postmortem human brain tissue from specialized brain banks, including those at the Department of Veterans Affairs and the Eunice Kennedy Shriver National Institute of Child Health and Human Development. This human tissue-based research, complemented by rigorous animal model studies, affords an unprecedented window into the neurobiological substrates of narcolepsy, transcending prior limitations inherent in solely rodent-based research paradigms.
The evidence of localized neuroinflammation and selective neuronal degeneration also invites a broader reconsideration of narcolepsy as a potential autoimmune or immune-mediated neurodegenerative disease. This perspective aligns with genetic and epidemiological data linking narcolepsy to specific HLA alleles and autoimmune disorders, suggesting that future research might focus on immunomodulatory therapies or neuroprotective strategies aimed at preserving both hypothalamic and brainstem neurons.
In conclusion, this seminal study overturns a quarter-century-old dogma by demonstrating that narcolepsy with cataplexy involves a dual degeneration of both hypocretin-producing neurons in the hypothalamus and norepinephrine-producing cells in the locus coeruleus. This dual-pathology paradigm offers a more nuanced understanding of the disorder, reconciles inconsistencies in clinical phenotyping, and opens transformative therapeutic possibilities. As we advance, integrating these insights into clinical practice and research agendas will be essential to fully unravel and effectively combat the complex neurobiology of narcolepsy.
Subject of Research: Human tissue samples
Article Title: Human narcolepsy is linked to degeneration of both locus coeruleus and hypocretin neurons
News Publication Date: 28-Mar-2026
Web References: https://www.nature.com/articles/s41467-026-70899-x
References: Article DOI: 10.1038/s41467-026-70899-x
Keywords: Narcolepsy, Cataplexy, Hypocretin neurons, Locus coeruleus, Norepinephrine, Neurodegeneration, Neuroinflammation, Microglia, Immune-mediated, Sleep disorders, Neurobiology, Brainstem
Tags: dual neuronal population involvement narcolepsyexcessive daytime sleepiness neurological causeshypocretin neuron degenerationlocus coeruleus role in narcolepsymuscle weaknessnarcolepsy with cataplexy researchneurodegeneration in hypothalamus and brainstemnorepinephrine synthesis in sleep disorderspathophysiology of narcolepsy type 1postmortem brain analysis narcolepsysevere narcolepsy brain damageUCLA narcolepsy study 2024