A recent cohort study published in JAMA Network Open sheds new light on the operational challenges and geographic disparities related to donor care units (DCUs) in the management of deceased donors after brain death. Despite broad consensus advocating for the benefits of DCUs and their implementation in clinical practice, the study highlights significant inefficiencies that impede optimal organ donation outcomes across the United States. This investigation prompts a reevaluation of current logistical frameworks, emphasizing system-wide reform to enhance organ transplantation efficiency and patient survival.
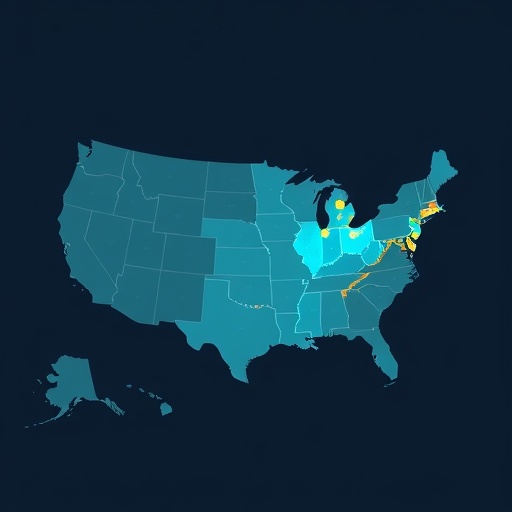
DCUs are specialized units designed to optimize the care of deceased donors, facilitating organ preservation, assessment, and eventual procurement. These units have garnered support for their ability to standardize donor management and improve transplantation success rates. However, this study reveals a heterogeneous adoption pattern across donation service areas (DSAs), unevenly distributing access to DCUs and thereby potentially compromising equitable organ donation opportunities. The uneven distribution means that a significant number of donors are located over a 180-minute drive from the nearest DCU, underscoring a critical geographic barrier.
The findings raise pressing concerns about the systemic boundaries currently defining organ procurement organizations (OPOs) and their operational reach. Donation service areas, which are typically delineated by regulatory and administrative borders, may unintentionally hamper the efficient placement and transfer of donors to the closest and most adequately equipped care units. This siloed approach may delay critical donor management interventions, reducing the viability of organs and diminishing overall transplantation outcomes.
Transportation logistics emerge as a critical focal point in this context. The study suggests that overcoming service area boundaries through innovative donor transport solutions could mitigate the current inefficiencies. By enabling cross-boundary transfer of donors to DCUs, healthcare systems might reduce time delays and enhance organ preservation quality. This approach would require coordination among regional OPOs, as well as investment in transport infrastructure and clinical protocols tailored for rapid donor movement.
Another solution proposed involves expanding the number of DCUs within acute care hospitals, thus reducing geographic gaps and shortening the time required for donor admission to specialized care. Integration of DCUs into existing hospital infrastructures presents challenges in resource allocation, staffing, and training but could yield significant gains in donor management quality and organ yield. The study calls for targeted policy initiatives and funding streams to incentivize such expansions, especially in underserved and rural areas.
Beyond logistical considerations, the study’s implications extend to ethical and clinical practices within transplant medicine. Ensuring equitable access to DCUs aligns with broader goals of fairness and maximizing life-saving opportunities through organ transplantation. Uneven DCU access risks perpetuating disparities among populations geographically distant from these units, potentially reflecting socioeconomic and demographic inequities. Addressing these gaps is therefore not only a clinical imperative but a public health and social justice concern.
Technological advances in remote donor monitoring and telemedicine integration may support overcoming geographic limitations, supplementing physical DCU presence by enabling expert consultation and real-time management guidance. These tools could facilitate earlier detection of donor instability and optimize protocols prior to transport or in smaller hospitals lacking dedicated DCUs. Incorporating such innovations may constitute another layer of intervention to complement infrastructural reforms.
The study’s rigorous cohort design strengthens the validity of its conclusions, drawing on comprehensive data sets that track donor locations, transport times, and DCU availability across multiple OPOs. This methodology allows for sophisticated spatial and temporal analyses, elucidating patterns that inform practical recommendations. The authors advocate for a system-level realignment to harness efficiencies, reduce organ loss, and ultimately save more recipient lives.
Regulatory reform may be a pivotal driver of change, aligning incentives for cross-boundary cooperation among OPOs and mandating minimum standards for DCU access. This could involve revising allocation policies, reimbursement models, and accountability frameworks to foster collaboration across traditional geographic lines. The study highlights that entrenched boundaries, while administratively convenient, may pose unnecessary barriers to the fluid management of donor resources.
In sum, this investigation provides a comprehensive appraisal of the structural and logistical challenges impacting donor care units and their role in deceased donor management. By recommending both the expansion of DCUs into acute care settings and innovative donor transport strategies that transcend donation service area boundaries, the study charts a forward path to enhance organ donation efficiency. Adoption of these measures would necessitate multifaceted collaboration among clinical providers, OPOs, policymakers, and health system leaders.
As the field continues to evolve toward optimizing organ transplantation outcomes, this study underscores the critical importance of addressing geography, infrastructure, and policy simultaneously. In doing so, it contributes a vital evidence base for engineering a more equitable, effective, and responsive organ donation system capable of meeting current and future demands.
Corresponding Author: Dr. Peter P. Reese can be contacted at [email protected] for further inquiries regarding the study findings and implications.
Subject of Research: Organ donation infrastructure and donor care unit accessibility
Article Title: [Not provided in the source]
News Publication Date: [Not provided in the source]
Web References: doi:10.1001/jamanetworkopen.2026.1703
Keywords: Organ donation, donor care units, brain death, donation service areas, deceased donors, transplant logistics, acute care hospitals, donor transport, health care system efficiency, geographical disparities, organ procurement organizations
Tags: brain death donor management efficiencydisparities in deceased donor managementdonation service area geographic disparitiesdonor care unit distribution in the USequitable access to donor care unitsgeographic accessibility to organ donor care unitsimpact of donor care units on organ transplantationimproving organ donation outcomeslogistical barriers in organ donationoptimizing deceased donor preservationorgan procurement organization operational challengessystem-wide reform in transplantation logistics